Our authors’ recent research shows that melanoma in situ, the earliest form of the disease, is on the rise, especially among young men. Here’s why this is bad news and good news, and what everyone (not just the men) needs to know to stay ahead of it.
By H. WILLIAM HIGGINS II, MD, MBE, and DAVID LEFFELL, MD
Growing up in Texas, Jim was no stranger to sun exposure. A year-round athlete, he also spent many summers landscaping, and he was proud of his golden bronze tan. To achieve this look, he purposely burned during his first intense sun exposure in spring, thinking that would be a good start on maintaining a tan through the summer. He even frequented tanning salons during the winter to keep it going.
When Jim’s mother noticed a spot on his cheek she’d never seen before, she pointed it out to him. It was dark brown, about the size of a pencil eraser, and it had an irregular shape. At first glance, it looked like a new freckle or mole. When it continued to grow, Jim became worried and visited a dermatologist. Just 29 years old, he was shocked when tests showed he had melanoma, a cancer that arises in the skin’s pigment-producing cells.
He was lucky, though. It was melanoma in situ: The tumor had not invaded beyond the epidermis, the outermost layer of the skin. The earliest form of melanoma (considered stage 0), it is the easiest to treat and almost always curable. If Jim had waited any longer before seeing the doctor, it could have been much worse.
Who’s at Risk
My colleagues and I have studied trends in melanoma in situ. Our 2015 report in the Journal of the American Academy of Dermatology found that over the past three decades, as the number of overall melanoma cases diagnosed steadily increased, melanoma in situ made up a large amount of this increase. We also noted a faster rate of increase in younger people ages 20 to 49 than in older people, and in men compared with women.
That means people like Jim. We share his story with you because we want everyone to be aware of the dangers of melanoma and how crucial early detection is. And we want to issue a special wakeup call to young people, whose melanoma incidence at all stages has been skyrocketing, and most of all, young men, who are notorious for staying away from doctors until faced with an emergency. There’s no such thing as a good melanoma, but the earlier you catch it, the better off you are.
In general, people who have red hair or light-colored skin, who have many moles, who tend to burn quickly in the sun, and who have had severe or blistering sunburns are at increased risk for melanoma in situ. There’s a genetic component as well, so the risk is also higher if you have an immediate family member with a history of melanoma.
What They Look Like
Melanomas in situ tend to be flat and asymmetric with irregular borders. They can be black, brown, tan, gray or even pink if the person has very fair skin. Areas that receive the greatest sun exposure, such as the scalp, face and neck, are more likely to develop melanoma in situ than the arms or legs. However, non-sun exposed areas, such as the buttocks, are also at risk. We don’t always understand the causes of these melanomas, though heredity can play a role. To detect melanoma in situ as early as possible, it helps to monitor your own skin. Head-to-toe self-examinations are a good place to start, including the areas where the sun doesn’t shine. When evaluating your skin, focus on the ABCDEs of melanoma detection. A stands for asymmetry; B for irregular borders; C for more than one color; D for diameter greater than 6mm (about ¼”), or the size of a pencil eraser; and E for evolving, meaning any lesion that is new or changing. View helpful photos showing the ABCDEs of melanoma.
Millimeters Matter
To diagnose melanoma in situ (or any melanoma), a doctor performs a biopsy on the suspicious spot, removing tissue and sending it to a lab to be interpreted by a qualified dermatopathologist. Jim’s diagnosis of melanoma in situ meant that surgery was all he needed. While surgery on the face is never good news, our research has shown that patients with melanoma in situ have the same life expectancy as the general population. However, we also know that people like Jim are at higher risk for developing future skin cancers, including more serious, invasive melanomas.
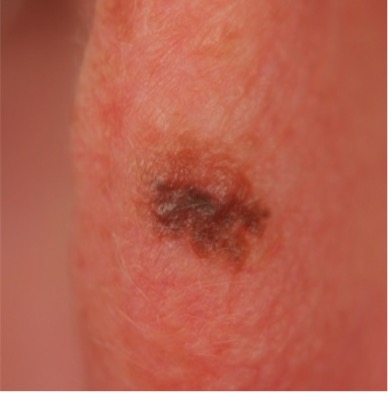
Stay on the Lookout – Melanomas in situ are usually flat and asymmetrical, with irregular borders. They can be black, brown, tan, gray or even pink.
In contrast to what Jim had, invasive melanomas are tumors that have penetrated beyond the epidermis into the deeper layer of the skin called the dermis. Melanoma is a battle of millimeters. In situ melanomas don’t spread to other parts of the body or cause death, but if the tumor has an opportunity to grow even one millimeter deep into the skin, it can lead to more involved treatment and greater danger. If left untreated, it can metastasize and even become life-threatening. Early detection can make all the difference.
Melanoma in situ is also associated with the development of additional cancers. These secondary tumors include lip cancer, Hodgkin lymphoma and leukemia/lymphoma. The average time to diagnosis of a secondary tumor is 14 years, which highlights the importance of regular follow-ups with your physician. For those who have a history of melanoma in situ, we recommend regular, professional full-body examinations at least once or twice a year. We also suggest checking your own skin head-to-toe once a month for any suspicious lesions. The same goes for anyone at higher risk of developing skin cancer.
Prevention
The best way to maintain healthy skin and help prevent melanoma in situ is to practice all-around sun protection. This includes seeking shade during the sun’s peak hours (10 AM to 4 PM), using SPF 15 or higher broad-spectrum sunscreen daily (SPF 30 or higher, water-resistant, broad-spectrum sunscreen for extended outdoor exposures) and wearing a wide-brimmed hat, UV-filtering sunglasses and other protective clothing. The sunscreen routine should include reapplying every two hours while active outdoors. View detailed tips on preventing skin cancer.
What’s the Takeaway?

Men in your 20s and 30s, we are especially talking to you. You’re in the group of people showing the fastest rise in the incidence of melanoma in situ. Step up and take precautions to avoid invasive melanoma, which will kill more than 10,000 people in the U.S. this year. Trust your instincts, and if you find any suspicious spot or new lesion, see a dermatologist immediately. When in doubt, check it out!
H. William Higgins II, MD, MBE, is an assistant professor, Department of Dermatology, Mohs Micrographic Surgery & Cutaneous Oncology, Alpert Medical School of Brown University, Providence, Rhode Island.
David J. Leffell, MD, is the David Paige Smith professor of dermatology, plastic surgery and otolaryngology, and section chief, Dermatologic Surgery and Cutaneous Oncology, Yale School of Medicine, New Haven, Connecticut. He is author of Total Skin and a former vice president of The Skin Cancer Foundation.
*This article was first published in the 2016 issue of The Skin Cancer Foundation Journal.





