World Congress on Cancers of the Skin
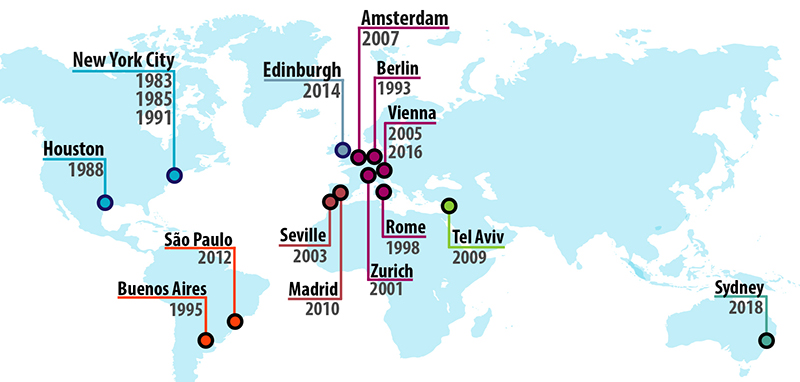
The The World Congress on Cancers of the Skin® is held in a different country every two years, and is sponsored jointly by The Skin Cancer Foundation and dermatological organizations from the host country. Since 1983 the Congress has enabled physicians to interact with distinguished international faculty and learn about breakthrough discoveries in the prevention, diagnosis, and treatment of all types of skin cancer.
The World Congress on Cancers of the Skin has become a major interdisciplinary and influential Congress for clinicians and basic scientists working in the challenging fields of melanoma and nonmelanoma skin cancer. This exciting Congress brings over 1,000 attendees together from around the world.