Basal Cell Carcinoma Treatment
Effective Options for Early and Advanced BCC
When detected early, most basal cell carcinomas (BCCs) can be treated and cured. Prompt treatment is vital, because as the tumor grows, it becomes more dangerous and potentially disfiguring, requiring more extensive treatment. Certain rare, aggressive forms can be fatal if not treated promptly.
If you’ve been diagnosed with a small or early BCC, a number of effective treatments can usually be performed on an outpatient basis, using a local anesthetic with minimal pain. Afterwards, most wounds can heal naturally, leaving minimal scarring.
Options include:
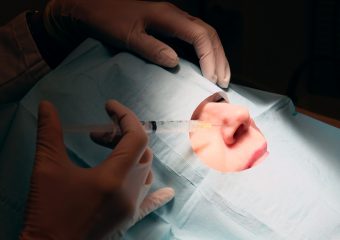
Mohs surgery
Curettage and electrodesiccation (electrosurgery)
How it works
The dermatologist scrapes or shaves off the BCC using a curette (a sharp instrument with a ring-shaped tip), then uses heat or a chemical agent to destroy remaining cancer cells, stop the bleeding and seal off the wound. The physician may repeat the procedure a few times during the same session until no cancer cells remain. Typically, the procedure leaves a round, whitish scar resembling a cigarette burn at the surgery site.
When it’s used
Curettage and electrodesiccation can be effective for most small BCC lesions. In these instances, the procedure has cure rates close to 95 percent.
Mohs surgery
How it works
Mohs surgery is performed during a single visit, in stages. The surgeon removes the visible tumor and a very small margin of tissue around and beneath the tumor site. The surgeon color-codes the tissue and draws a map correlated to the patient’s surgical site. In an on-site lab, the surgeon examines the tissue under a microscope to see if any cancer cells remain. If so, the surgeon returns to the patient and removes more tissue exactly where the cancer cells are. The doctor repeats this process until there is no evidence of cancer. Then the wound may be closed or, in some cases, allowed to heal on its own.
When it’s used
Mohs surgery is the gold standard, the most effective technique for removing BCCs, harming minimal healthy tissue while achieving the highest possible cure rate — up to 99 percent on tumors treated for the first time. It is often recommended for BCCs located in areas around the eyes, nose, lips, ears, scalp, fingers, toes or genitals. Mohs is also used for BCCs that are large, aggressive or growing rapidly and on tumors that have returned, as well as ones with indistinct edges. Get more details about Mohs surgery here.
Excisional surgery
How it works
Using a scalpel, the surgeon removes the entire tumor along with a “safety margin” of surrounding tissue and sends it to an off-site lab for analysis. The margin of skin removed depends on the thickness and location of the tumor. If the lab finds cancer cells beyond the margins, more surgery may be performed at a later date until margins are cancer-free.
When it’s used
For small, early BCCs that have not spread, excisional surgery is frequently the only treatment required. Cure rates are above 95 percent in most body areas, similar to those of curettage and electrodesiccation.
Radiation therapy
How it works
The physician uses low-energy X-ray beams to destroy the tumor, with no need for cutting or anesthesia. Destruction of the tumor may require several treatments over a few weeks or daily treatments for a specified time.
When it’s used
With radiation therapy, there is no way of knowing that all of the tumor was destroyed. Since the procedure is less precise and produces cure rates of only 90 percent, it is primarily used for BCCs that are hard to treat with surgery, and in elderly patients or people in poor health for whom surgery is not advised. For some cases of advanced BCC, especially those involving surrounding nerves, radiation may be used after surgery or in combination with other treatments.
Cryosurgery
How it works
The dermatologist uses a cotton-tipped applicator or spray device to apply liquid nitrogen to freeze and destroy the tumor. Later, the lesion and surrounding skin may blister or become crusted and fall off, allowing healthy skin to emerge.
When it’s used
Cryosurgery is effective for smaller, superficial BCCs. It is especially useful for patients with bleeding disorders or problems tolerating anesthesia. The cure rate is between 85 and 90 percent. This technique is used less commonly for invasive BCC because it may miss deeper portions of the tumor, and because scar tissue at the site can make a recurrence harder to detect.
Laser surgery
How it works
The dermatologist directs a beam of intense light at the tumor to target superficial BCCs. Some lasers vaporize (ablate) the skin cancer while others (nonablative lasers) convert the beam of light to heat, which destroys the tumor without injuring the surface of the skin.
When it’s used
Laser surgery is not yet FDA-approved for superficial BCCs but is sometimes used as a secondary therapy, especially when other techniques have been unsuccessful.
Photodynamic therapy (PDT)
How it works
The dermatologist applies a topical agent to make the lesion sensitive to light, or injects the agent into the tumor. After allowing a short period of time for absorption, the dermatologist uses a blue light or pulsed-dye laser (or sometimes controlled natural sunlight), which causes a reaction that destroys the BCC. After the procedure, patients must strictly avoid sunlight for at least 48 hours, as UV exposure will increase activation of the medication and may cause severe sunburns.
When it’s used
PDT can be used for some superficial BCCs on the face and scalp but is not recommended for invasive BCC.
Topical medications
Approved medications
5-fluorouracil (5-FU) (Efudex®, Carac®, Fluoroplex®, Tolak®)
Imiquimod (Aldara®, Zyclara®)
How they work
These are creams or gels applied directly to affected areas of the skin to treat superficial BCCs with minimal risk of scarring. Imiquimod activates the immune system to attack cancerous cells, while 5-FU is a topical chemotherapy that kills cancerous cells.
When they are used
5-FU, a chemotherapy approved to treat certain internal cancers, has also been FDA-approved in topical form for superficial BCCs, with cure rates between 80 and 90 percent. Imiquimod is approved for superficial BCCs, with cure rates between 80 and 90 percent. Oftentimes tumors diagnosed on biopsy to be superficial will have other invasive areas within the same lesion, making appropriate tumor selection for this treatment intrinsically difficult.
When weighing the pros and cons of treatment options, it’s important to consider that radiation, cryosurgery and topical medications all have one significant drawback in common — no tissue is examined under the microscope, so there is no way to determine how completely the tumor was removed.
Treating advanced BCCs
Approved oral medications
Two oral medications are FDA-approved for treating adults with very rare cases of advanced BCC that are large or have penetrated the skin deeply, spread to other parts of the body or resisted multiple treatments and recurred.
Vismodegib (Erivedge®)
Sonidegib (Odomzo®)
How they work
Both medications are targeted drugs taken by mouth. They work by blocking the “hedgehog” signaling pathway, a key factor in the development of BCC. In 2012, vismodegib became the first medicine ever approved by the FDA for treating advanced BCC. A second hedgehog pathway inhibitor (HHI) drug, sonidegib, was approved for advanced BCC in 2015.
When they are used
Vismodegib is used for the extraordinarily rare cases of metastatic BCC or locally advanced BCC (tumors that have penetrated the skin deeply or frequently recurred) that either recur after surgery or radiation, or cannot be treated with surgery or radiation and have become dangerous or life-threatening.
Sonidegib is used in adults with BCC that is locally advanced, penetrating the skin deeply or repeatedly recurring, as well as in cases when other treatments such as surgery or radiation cannot be used.
Due to a risk of birth defects, women who are pregnant or may become pregnant should not use either drug. Couples must use birth control if the woman is capable of becoming pregnant while her partner is taking the medication.
Scientists are also investigating several other targeted hedgehog inhibitors as potential treatments for locally advanced and metastatic BCC.
Approved immunotherapy medications
In February 2021, the U.S. Food and Drug Administration (FDA) approved the intravenous immunotherapy medication, cemiplimab-rwlc (Libtayo®) for treating patients with certain forms of advanced basal cell carcinoma.
Cemiplimab-rwlc (Libtayo®)
How it works
Cemiplimab is a type of immunotherapy known as a checkpoint blockade therapy, which works by harnessing the power of the immune system to battle cancer. Under normal conditions, the immune system uses checkpoints, which are molecules that suppress production of T cells, the white blood cells that help protect the body from infection. These checkpoints keep T cells from overproducing and attacking normal cells in the body. However, cancer cells have the ability to keep those checkpoints active, suppressing the immune system so the cancer can grow and thrive. Cemiplimab blocks a particular checkpoint called PD-1 from working, so the immune system can release massive amounts of T cells to attack and kill cancer cells.
Find out more about cemiplimab.
When it’s used
Cemiplimab is used to treat patients with advanced basal cell carcinoma (BCC) previously treated with a hedgehog pathway inhibitor (HHI) or for whom an HHI is not appropriate. Full approval was granted for patients with locally advanced BCC and accelerated approval was granted for patients with metastatic BCC.
Reviewed by:
Julie K. Karen, MD
Ronald L. Moy, MD
Last updated: April 2021
Note: The information included on this website is medically reviewed and factually accurate. It is intended for educational purposes only. The treatment information on this page is not a recommendation or endorsement of any drug, device or treatment, nor does it suggest that any drug, device or treatment is safe or effective for you. If you have any questions about skin cancer treatments, please talk to your health care provider.
