Rare Skin Cancers
What You Need to Know About Uncommon Skin Diseases
While basal cell carcinoma, squamous cell carcinoma and melanoma are more widespread, these rare skin cancers are important to know about, because they may be mistaken for noncancerous conditions, delaying diagnosis and treatment.
Types of Skin Cancer
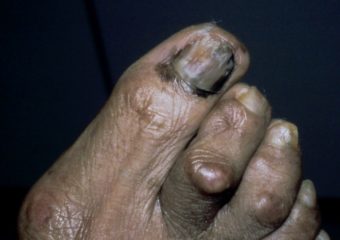
Acral lentiginous melanoma
What is it? Acral lentiginous melanoma (ALM) is a very rare, aggressive type of skin cancer. While uncommon in general, ALM is the most common type of melanoma found in people of color, including individuals of African ancestry.
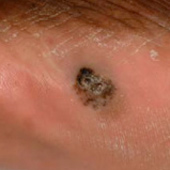
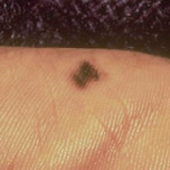
What does it look like? ALM may appear as a black or brown area of skin, in hard-to-spot places including under the nails (subungual) and on the soles of the feet or palms of the hands.
What causes it? While most melanomas are caused by exposure to ultraviolet (UV) radiation from the sun or from tanning beds, ALM, which develops on hairless skin, is more likely caused by genetic factors.
How is it treated? Excisional surgery is usually performed to remove the primary tumor and a margin of healthy tissue around it. Depending on the size and location of the tumor, and the overall health of the patient, other treatment options include radiation therapy, immunotherapy, targeted therapy and chemotherapy. The five-year survival rate for African American patients with melanoma is 71 percent. Most deaths from this form of melanoma occur when it is diagnosed late, after it has begun to spread.
Photo credit: Hugh Gloster, MD
Cutaneous T-cell lymphoma
What is it? Cutaneous T-cell lymphoma (CTCL) is a rare type of blood cancer that arises on the skin. CTCL starts in white blood cells called T-lymphocytes that normally fight infection in the body. The most common subtype is known as mycosis fungoides (MF), which is more prevalent among Black people than it is among other racial groups. Sézary syndrome is a less common but more aggressive subtype that may appear as an intense, widespread red rash over the body.
What does it look like? T-cell lymphoma most commonly affects the skin, causing rash-like patches or plaques that grow or spread, itching, lumps on the skin and sometimes even tumors. The disease can also involve the blood, lymph nodes and internal organs. It can be difficult to identify and may require multiple biopsies at different stages of development to get a correct diagnosis.
What causes it? The cause of cutaneous T-cell lymphoma is not known. What scientists do know is that the disease begins when T-cells develop changes (mutations) in their DNA causing them to mutate, grow rapidly and attack the skin.
How is it treated? While T-cell lymphoma is not curable, symptoms can be controlled and treated in the following ways:
- Topical medications, including steroids, retinoids and chemotherapy.
- Phototherapy, where physicians use special devices to treat the skin with targeted doses of ultraviolet light.
- Radiation therapy, specifically electronic beam therapy.
Dermatofibrosarcoma protuberans (DFSP)
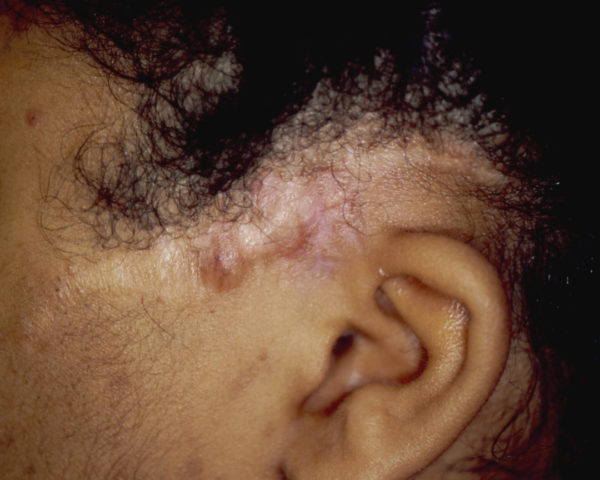
What is it? Unlike common skin cancers that arise from cells in the outermost layer of skin, dermatofibrosarcoma protuberans (DFSP) is an extremely rare cancer that arises from cells in the deepest layer of the skin, known as the dermis. While DFSP is slow growing and rarely spreads (metastasizes) to distant areas of the body, it has a high rate of local recurrence.
What does it look like? DFSP can look like an ordinary scar, cyst or bruise. It can develop anywhere on the body but is most commonly found on the arms, legs or torso. Over time, it can grow to become a large lump under the skin. The tumor grows slowly but can penetrate deep into the dermis and infiltrate the fat and surrounding tissue.
What causes it? Experts do not fully understand what causes DFSP, but injuries to the affected skin may be a risk factor.
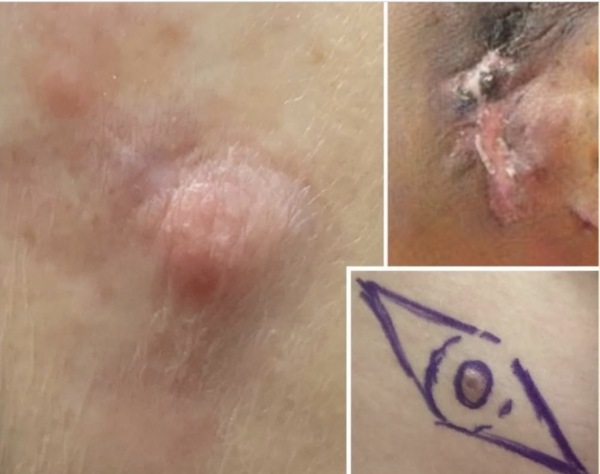
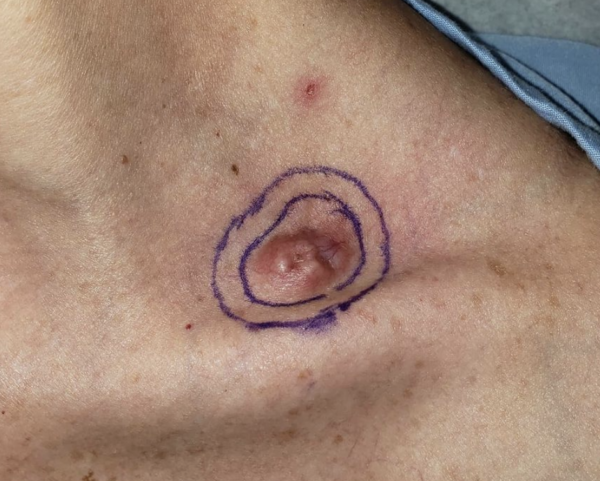
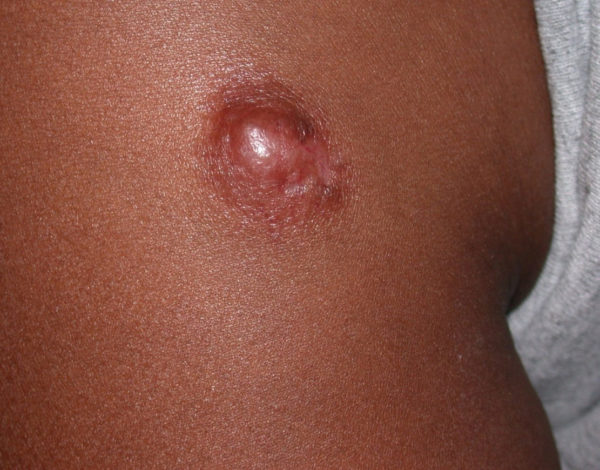
How is it treated? DFSP is often treated by excisional surgery to remove the tumor and a margin of healthy skin. Additional treatments include:
- Mohs surgery: This specialized surgery involves removing and assessing layers of the tumor until only cancer-free tissue remains. This procedure produces the highest cure rate for DFSP and spares the most amount of healthy tissue. More about Mohs surgery.
- Radiation therapy: Radiation destroys cancer cells when surgery is not an option or if DFSP recurs after surgery.
- Targeted therapy: Drugs like imatinib (Gleevac) that target and attack certain cells have been approved by the FDA to treat DFSP.
Kaposi’s sarcoma
What is it? Kaposi’s sarcoma is a rare skin cancer that develops from the cells that line the blood vessels or lymph vessels. There are two types of Kaposi’s sarcoma:
- The first type, often referred to as classic Kaposi’s sarcoma (CKS) is often seen in men over age 50 of European, Mediterranean or Middle Eastern descent. This type is slow growing, easier to treat and rarely causes serious problems.
- The second type is an aggressive cancer that affects people with weakened immune systems, including cancer patients, organ transplant recipients and people who are HIV positive. While this dangerous, fast-growing cancer is on the decline thanks to antiviral medications, if you think you may be at risk, get prompt medical attention.
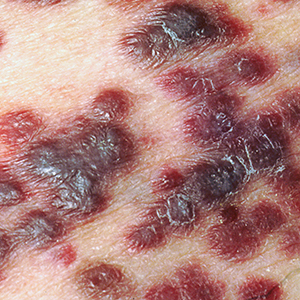
What does it look like? Kaposi’s sarcoma can present as red, purple or brown lesions on the skin, mucous membranes, lymph nodes and other organs. The lesions may be flat or slightly raised and can grow and spread rapidly.
Photo credit: ALAMY
What causes it? The disease is caused by the Kaposi’s sarcoma associated herpesvirus 8 (KSHV). People with healthy immune systems can be exposed to the virus and show little or no signs or symptoms, because of the immune system’s ability to keep the virus in check. Cancer patients receiving chemotherapy, HIV positive patients and organ transplant patients are all at a high risk of serious infection. The virus is believed to be transmitted by the exchange of saliva.
How is it treated? Kaposi’s sarcoma can be treated in several different ways depending on the stage of the disease and the overall health of the patient. Treatment options include:
Excisional surgery
Mohs surgery
Cryosurgery
Chemotherapy
Antiviral therapy
Immunotherapy
Radiation therapy
The more serious form of Kaposi’s sarcoma is treated mainly by systemic antiviral therapy to kill the virus that is causing the disease.
Microcystic adnexal carcinoma
What is it? Microcystic adnexal carcinoma (MAC) is a very rare tumor of the skin that develops in the sweat gland, most often in the head and neck region. This type of tumor is also known as a sclerosis sweat gland carcinoma. Although MACs may occur in other parts of the body, they commonly present on sun exposed areas in the middle of the face. People ages 50 and older are most likely to develop these tumors. While MACs can be locally aggressive, growing in size and into nearby tissues, they rarely spread (metastasize) to more distant parts of the body.
What does it look like: MAC can appear as a yellowish spot, raised patch or smooth bump on the skin.
What causes it: The cause of microcystic adenexal carcinoma is not yet known. Risk factors include exposure to ultraviolet light (UV) light from the sun, radiation treatment and immunosuppression.
How is it treated? Most MACs are treated with Mohs surgery.
Merkel cell carcinoma (MCC)
What is it? Merkel cell carcinoma (MCC) is a rare, aggressive skin cancer with a high risk for recurring and spreading (metastasizing) to other areas of the body. Merkel cells are located deep in the top layer of skin. Merkel cells are connected to nerves, signaling touch sensation as “touch receptors.” MCC was named after Merkel cells due to the similar microscopic features; however, recent research suggests that it is unlikely that MCC originates directly from normal Merkel cells.
Learn more about MCC
Visit our MCC Patient Support Center
View photos of MCC
What causes it? Evidence of the Merkel cell polyomavirus can be found in most, but not all, Merkel cell tumors. Since it’s a common virus and MCC is a rare disease, scientists are not certain about how or why the virus causes MCC in some people. What is clear is that factors such as UV exposure and immunosuppression also play a role.
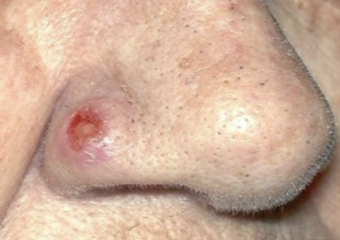
What does it look like? These tumors usually appear as firm, painless lesions or nodules on sun-exposed areas of the body, including the head, neck or eyelids. While these tumors are not as distinctive as other skin cancers, their rapid rate of growth is often what causes patients and doctors to take notice.
How is it treated? MCC treatment options are determined by the stage of the disease and the overall health of the patient. Treatment includes surgical removal of the primary tumor along with:
Sebaceous carcinoma
What is it? A sebaceous carcinoma is an uncommon cancer that arises from the unchecked growth of cells that line the oil glands (sebaceous glands or sebum-producing glands) in the skin. It often develops on the face and eyelids, but can occur anywhere on the body. According to the American College of Mohs Surgery, about thirty percent of people with a genetic condition known as Muir-Torre syndrome develop sebaceous carcinomas. Patients with Muir-Torre syndrome can also develop internal malignancies, including colon cancer.
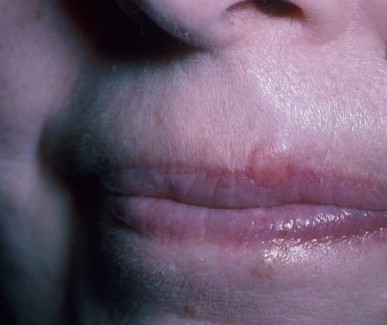
What does it look like? The tumor may arise as a lump or thickening of the skin on the eyelid or on the face that is often painless, and sometimes oozes or bleeds. In other parts of the body, the tumor may look like a yellowish lump which sometimes bleeds.
Photo credit: Ramin Fathi, MD and Stan Tolkachjov, MD, FACMS via ACMS
How is it treated?
Undifferentiated pleomorphic sarcoma
What is it? Undifferentiated pleomorphic sarcomas are rare soft tissue tumors that often arise from cells known as fibroblasts, in the dermis. This type of tumor often occurs in older men. Undifferentiated pleomorphic sarcomas can occur anywhere on the body. They can grow quickly and spread to other parts of the body. Superficial tumors were once known as atypical fibroxanthomas, and deeper, more advanced tumors were called malignant fibrous histiocytomas.
What does it look like? A growing lump or area of swelling on the skin that appears on the arms, legs, abdomen or scalp.
How is it treated? Surgery is usually performed to remove the primary tumor. Depending on the size and location of the tumor, and the overall health of the patient, other treatment options include Mohs surgery, radiation therapy, chemotherapy and immunotherapy.
Extramammary Paget's disease (EMPD)
Extramammary Paget’s disease (EPMD) is a rare disease that frequently presents in areas where apocrine sweat glands are abundant, in the armpits or around the anus and genitals. The condition is related to Paget’s disease of the breast. This very slow-growing cancer sometimes takes years to become noticeable.
What does it look like? A persistent, sometimes irritating rash that resembles eczema and does not respond to topical treatments.
How is it treated?