Your eyes can focus on a tiny splinter in the finger of a squirming child, a stop sign in the distance or stars blinking light-years away. You can roll your eyes, flirt with them, do a double-take and express joy or despair without words. When you think about how amazing your eyes are, wouldn’t you do anything to protect them?
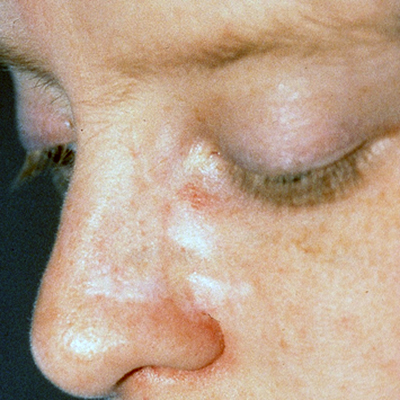
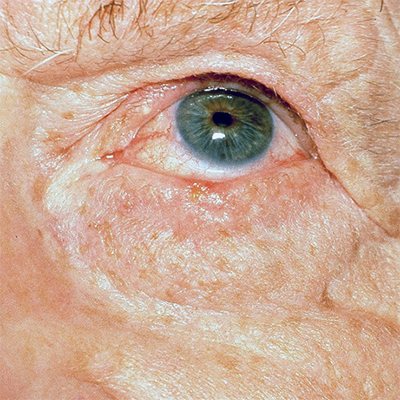
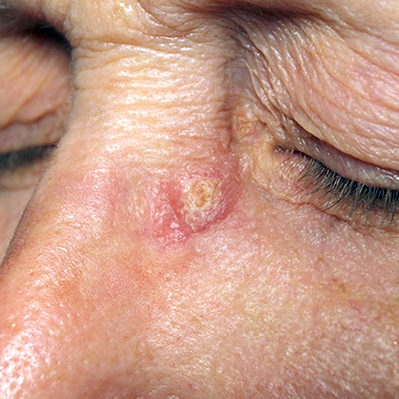
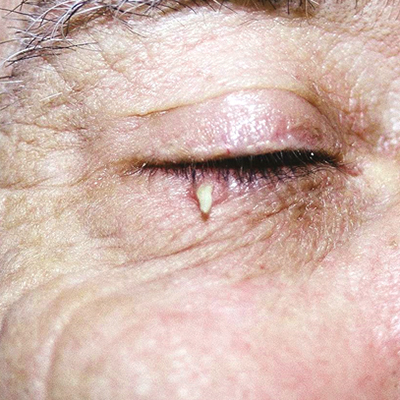
Strong bony sockets called orbits encase and safeguard your eyes. The thin tissue surrounding them, however, including your upper and lower eyelids, is extremely vulnerable to damage from the sun’s ultraviolet rays. Because of that, nonmelanoma skin cancers on and around the eyelids are common.
A big hat and UV-blocking sunglasses can help, and so can sunscreen — if you actually use it around your eyes. Many people stop short of the eye area when applying products, mainly because of sensitivity concerns. Even among those who use sunscreen on their faces regularly, the most often-missed spots are around the eyelids, according to a small British study. For advice on what type of sunscreen to use around your eyes, see this “Ask the Expert” article.
Have You Been Diagnosed?
The vast majority of skin cancers around the eyes are basal cell carcinomas (BCCs). While BCCs rarely spread to the lymph nodes or beyond, they can grow large enough to cause disfigurement around your eyes. Squamous cell carcinomas (SCCs) account for a small percentage of eyelid cancers. This type has a higher chance of spreading and, in a small number of cases, may become life-threatening. Melanoma, a more dangerous form of skin cancer, can occur around and in the eye, but it is far more rare.
If you’ve just been diagnosed with a nonmelanoma skin cancer near your eye, it may seem scary, but don’t panic, says New York City dermatologist and Mohs surgeon Désirée Ratner, MD. “This is such a common location to develop skin cancers, and dermatologic surgeons know how to manage them. Even though you might feel freaked out, for us it’s routine.”
Treatment of Choice
Mohs surgery is the treatment of choice for most nonmelanoma skin cancers near the eyes. Specially trained dermatologic surgeons do this procedure in stages, while the patient waits between each stage. After removing a layer of tissue, the Mohs surgeon examines 100 percent of the tumor margins under a microscope in an on-site lab. If any cancer cells remain, the surgeon knows where they are and removes another layer of tissue only from that precise location, then performs the lab work on that specimen. The doctor repeats this process until no cancer cells remain. This technique has very high cure rates, spares the greatest amount of healthy tissue and leaves the smallest scar possible.
Even if you’ve had previous skin cancer treatment, you might feel squeamish about having surgery near your eyes, says Dr. Ratner. She wants to calm your fears. “During Mohs surgery, I’m able to do most of it with the patients’ eyes closed, so they don’t have to see what’s going on,” she says. “If the tumor is right on the eyelid margin, I put a numbing drop in that eye and then insert an opaque contact lens. That lets patients open their eyes comfortably while I’m working.”
Once the lab work shows that there are no more cancer cells, the surgeon closes the wound. Frequently there is a way to stitch the edges together along a natural line around the eye, so once it heals it will barely be visible. Your scar might end up a little longer than you would have thought, but for good reason. “Sometimes, in pushing the edges of the skin together,” Dr. Ratner explains, “extra tissue needs to be removed to avoid a pucker or a lump that would distract from an otherwise elegant repair.”
Occasionally, a Mohs surgeon might work with a specialist on the wound repair. “If the skin cancer is near the tear duct, on the lid margin or is very large, before I do the surgery I might refer the patient for a consultation with an oculoplastic surgeon (an ophthalmologist who specializes in plastic surgery around the eyes). Then, on the day of surgery, the oculoplastic surgeon performs the closure after I’ve removed the cancer.”
Recovery After Eyelid Surgery
Some patients may need to wear an eye patch for a few days. Swelling and bruising are common after surgery around the eyes. “I tell all my patients who have surgery near the eye that they’ll probably have a black eye afterwards. If they don’t, they’ll be pleasantly surprised. If the surgery was on the upper eyelid, I warn them that it may swell shut. Sleeping with the head elevated can help.” And thanks to gravity, swelling goes away fairly quickly within a few days.
It takes six months to a year for a scar to heal completely, Dr. Ratner explains. “Some patients may develop a hypertrophic, or raised, scar, especially on the lower eyelids, because when you blink or raise your eyebrows, the body feels that tension and pulls back. But we have procedures, such as steroid injections, that can flatten out thickened scars if they become uncomfortable or noticeable.”
Warning Signs of Skin Cancer on the Eyelids