Merkel Cell Carcinoma Overview
A Rare, Aggressive Skin Cancer
Merkel cell carcinoma (MCC) is a rare, aggressive form of skin cancer with a high risk for returning (recurring) and spreading (metastasizing), often within two to three years after initial diagnosis.
How rare is it? Approximately 3,000 new cases of Merkel cell skin cancer are diagnosed annually in the U.S. About 40 percent of cases recur. Fortunately, options for managing recurrent disease have increased markedly with the introduction of immunotherapy treatments.
Merkel cell carcinoma (MCC) is 40 times more rare than melanoma, with an estimated one case per 130,000 people in the U.S.
Risk factors for MCC include sun exposure, light skin, age over 50 and a weakened immune system.
Singer-songwriter Jimmy Buffett battled MCC for four years prior to passing away on September 1, 2023. Buffett continued to perform throughout treatment for the disease before his death at age 76.
What is a Merkel cell?
Merkel cells are located deep in the top layer of skin. Merkel cells are connected to nerves, signaling touch sensation as “touch receptors.” MCC was named after Merkel cells due to the similar microscopic features; however, recent research suggests that it is unlikely that MCC originates directly from normal Merkel cells.
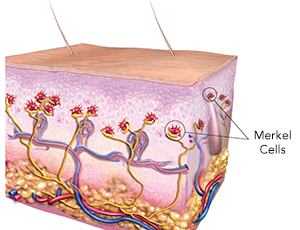
Normal Merkel cells in the skin: In this illustration of a cross-section of the skin, normal Merkel cells are shown in red and connect to nerves shown in yellow. The structures drawn include the epidermis (upper third), dermis (middle), and deeper adipose layer containing the fatty tissue. Arteries are depicted in red and veins are blue. Figure copyright by Paul Nghiem & Quade Medical Group.
What does MCC look like?
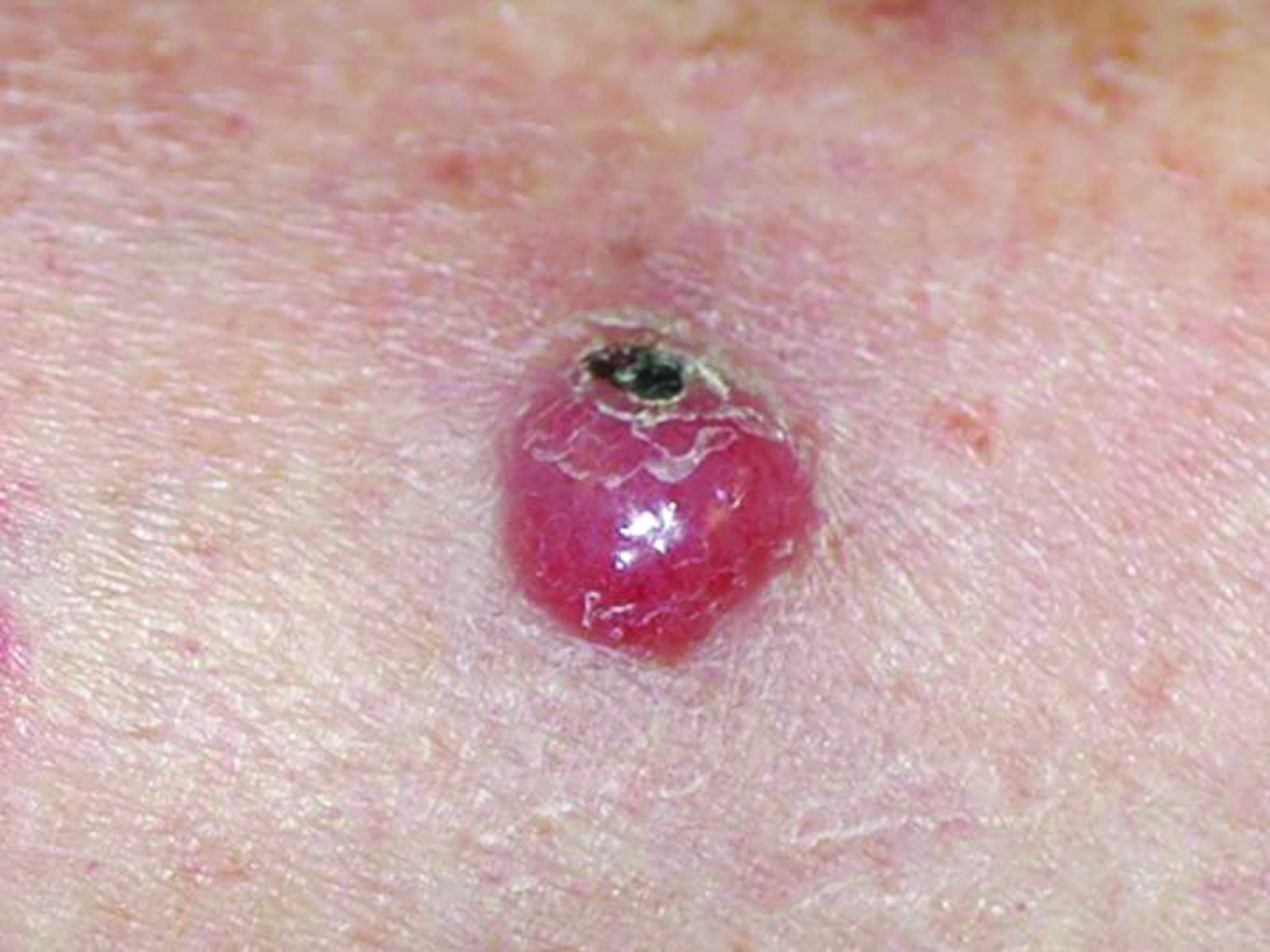
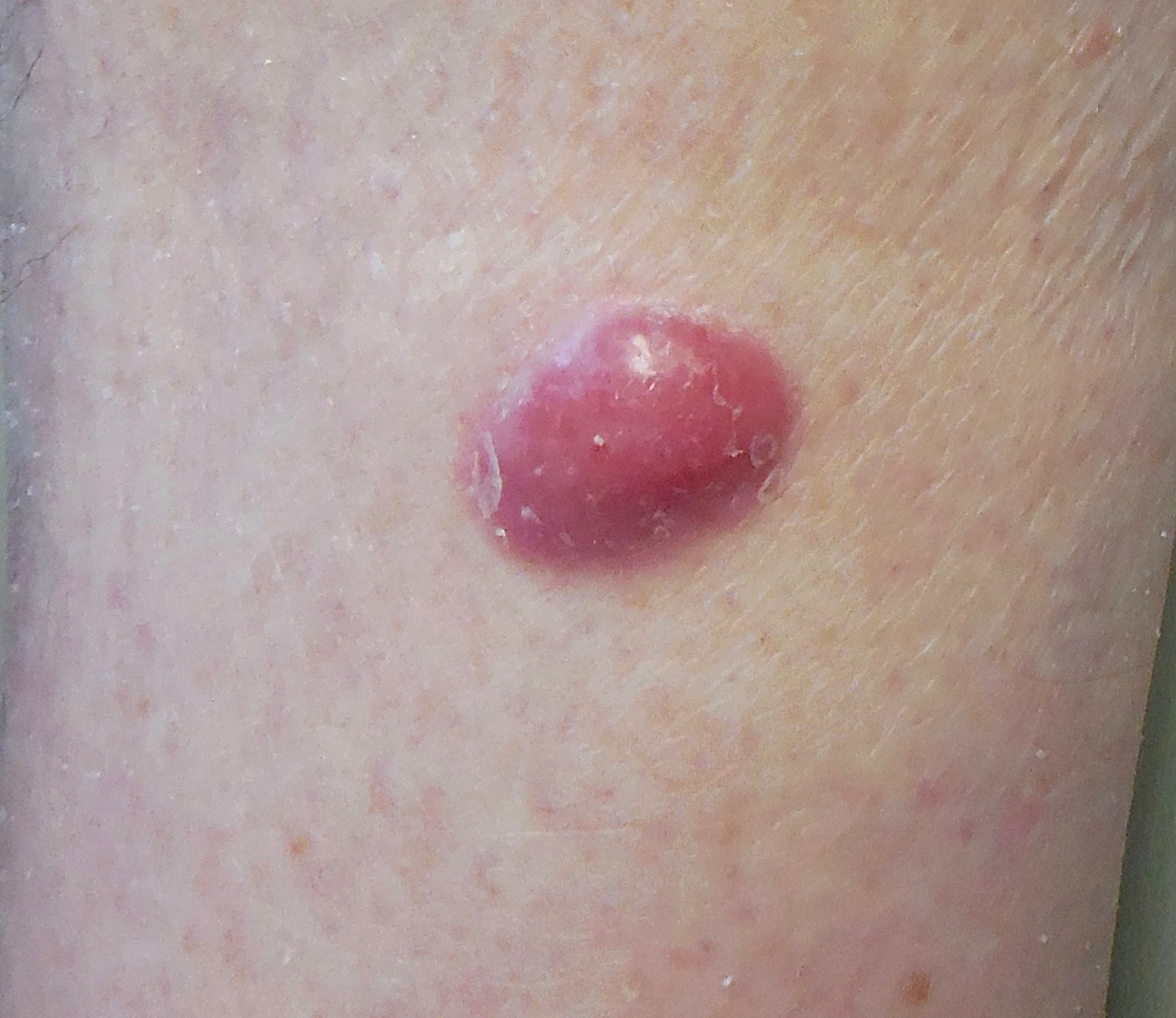
MCC tumors often, but not always, appear on sun-exposed areas of the body. The tumors are not nearly as distinctive as other skin cancers and can appear as a pearly pimple-like lump, sometimes skin-colored, red, purple or bluish-red, though they are rarely tender to the touch. The rapid speed at which they grow is what often causes patients and doctors to take notice.
Please note: Since not all Merkel cell carcinomas have the same appearance, these photos serve as a general reference for what MCC can look like. If you see something new, changing or unusual on your skin, schedule an appointment with your doctor. Photos courtesy of Paul Nghiem, MD, PhD
How dangerous is MCC?
While MCC is about three to five times more likely to be deadly than melanoma, with early detection, MCC can be treated successfully. If you think you might have MCC, see your doctor. Treatment becomes increasingly difficult once the disease has spread, but new options are now available. Thanks to advances in the field of immunotherapy, MCC survival rates are improving.
A survivor's story
When Luis found out he had Merkel cell carcinoma, a rare form of skin cancer, he was determined to beat it. He shares his harrowing journey from diagnosis to treatment.
Reviewed by:
Sandra D’Angelo, MD
Paul Nghiem, MD, PhD
Last updated: September 2023