Mohs Surgery
The Most Effective Technique for Treating Common Skin Cancers
Mohs surgery is considered the most effective technique for treating many basal cell carcinomas (BCCs) and squamous cell carcinomas (SCCs), the two most common types of skin cancer. Sometimes called Mohs micrographic surgery, the procedure is done in stages, including lab work, while the patient waits. This allows the removal of all cancerous cells for the highest cure rate while sparing healthy tissue and leaving the smallest possible scar.
It began as a technique called chemosurgery, developed by Frederic E. Mohs, MD, in the late 1930s, but was not widely known. In the mid 1960s, Perry Robins, MD, studied the procedure with Dr. Mohs, and recognized that it had great potential for the field of dermatology. He brought the technique to NYU, where he established the first fellowship training program to teach dermatologists this skin cancer surgery. Dr. Robins helped advance the procedure into what is now called Mohs surgery and went on to teach and promote it around the world.
The Advantage of Mohs
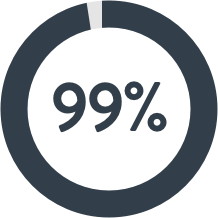
CURE RATE
for a skin cancer that has not been treated before
Who performs the procedure?
Mohs surgery is performed by doctors who are specially trained to fulfill three roles:
- as the surgeon who removes the cancerous tissue
- as the pathologist who analyzes the lab specimens
- as the surgeon who closes or reconstructs the wound
Advantages of Mohs surgery
Efficient, cost-effective treatment
- Single-visit outpatient surgery
- Local anesthesia
- Lab work done on-site
Precise results
- Physician examines 100% of tumor margins
- Spares healthy tissue
- Leaves the smallest scar possible
The highest cure rate
- Up to 99% for a skin cancer that has not been treated before
- Up to 94% for a skin cancer that has recurred after previous treatment
What happens during Mohs surgery
The procedure is done in stages, all in one visit, while the patient waits between each stage. After removing a layer of tissue, the surgeon examines it under a microscope in an on-site lab. If any cancer cells remain, the surgeon knows the exact area where they are and removes another layer of tissue from that precise location, while sparing as much healthy tissue as possible. The doctor repeats this process until no cancer cells remain.
Step 1: Examination and prep
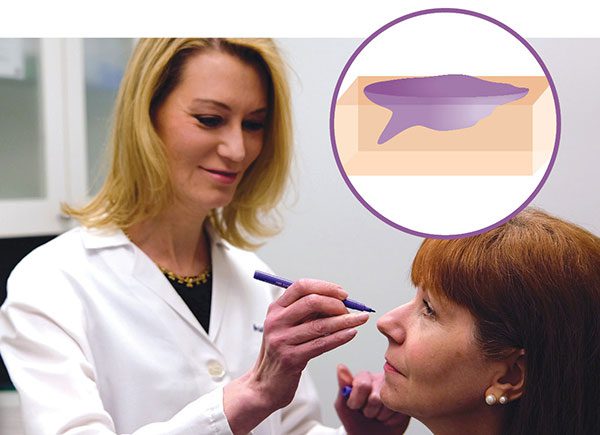 Depending on the location of your skin cancer, you may be able to wear your street clothes, or you may need to put on a hospital gown. The Mohs surgeon examines the spot where you had your biopsy and may mark it with a pen for reference. The doctor positions you for best access, which may mean sitting up or lying down. A surgical drape is placed over the area. If your skin cancer is on your face, that may mean you can’t see what’s happening, but the doctor talks you through it. The surgeon then injects a local anesthesia, which numbs the area completely. You stay awake throughout the procedure.
Depending on the location of your skin cancer, you may be able to wear your street clothes, or you may need to put on a hospital gown. The Mohs surgeon examines the spot where you had your biopsy and may mark it with a pen for reference. The doctor positions you for best access, which may mean sitting up or lying down. A surgical drape is placed over the area. If your skin cancer is on your face, that may mean you can’t see what’s happening, but the doctor talks you through it. The surgeon then injects a local anesthesia, which numbs the area completely. You stay awake throughout the procedure.
Step 2: Top layer removal
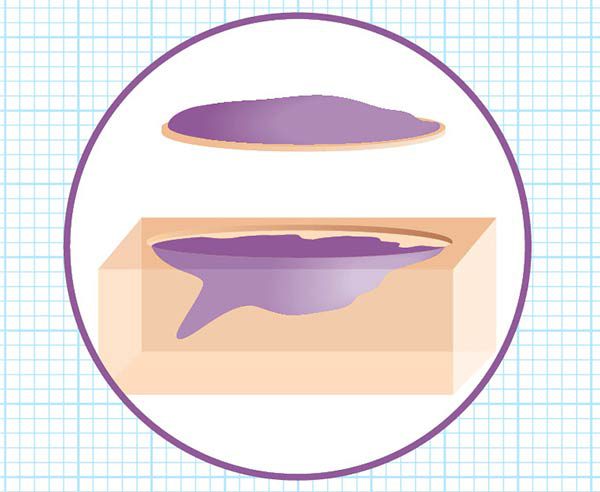 Using a scalpel, the surgeon removes a thin layer of visible cancerous tissue. Some skin cancers may be “the tip of the iceberg,” meaning they have roots or extensions that aren’t visible from the surface. The lab analysis, which comes next, will determine that. Your wound is bandaged temporarily and you can relax while the lab work begins.
Using a scalpel, the surgeon removes a thin layer of visible cancerous tissue. Some skin cancers may be “the tip of the iceberg,” meaning they have roots or extensions that aren’t visible from the surface. The lab analysis, which comes next, will determine that. Your wound is bandaged temporarily and you can relax while the lab work begins.
Step 3: Lab analysis
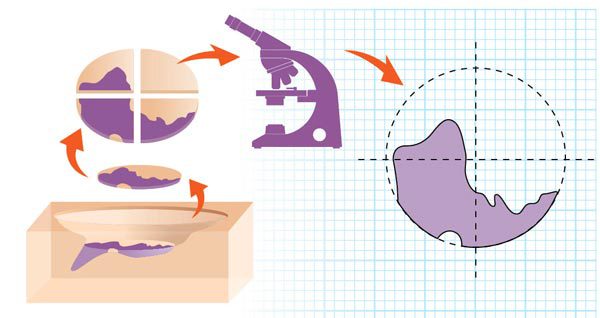 The surgeon cuts the tissue into sections, color codes them with dyes and draws a map of the surgical site. In the lab, a technician freezes the divided tissue, then cuts very thin horizontal slices like a layer cake. The slices are placed on microscope slides, stained and covered. This meticulous process takes time.
The surgeon cuts the tissue into sections, color codes them with dyes and draws a map of the surgical site. In the lab, a technician freezes the divided tissue, then cuts very thin horizontal slices like a layer cake. The slices are placed on microscope slides, stained and covered. This meticulous process takes time.
Step 4: Microscopic examination
Using a microscope, the surgeon examines all the edges and underside of the tissue on the slides and, if any cancer cells remain, marks their location on the map. The physician then lets you know whether you need another layer of tissue removed.
Step 5: Second layer removal
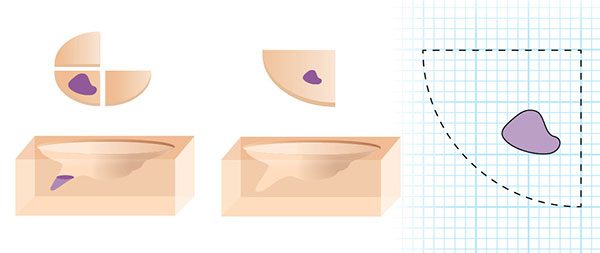 Back in the operating room, the surgeon injects more anesthesia if needed and removes another layer of skin, precisely where the cancer cells remain, based on the map. Then, while you wait, the lab work begins again. This entire process is repeated as many times as needed until there are no more cancer cells.
Back in the operating room, the surgeon injects more anesthesia if needed and removes another layer of skin, precisely where the cancer cells remain, based on the map. Then, while you wait, the lab work begins again. This entire process is repeated as many times as needed until there are no more cancer cells.
Step 6: Wound repair
Once the site is clear of all cancer cells, the wound may be left open to heal or the surgeon may close it with stitches. This depends on its size and location. In some cases, a wound may need reconstruction with a skin flap, where neighboring tissue is moved into the wound, or possibly a skin graft. In some cases, your Mohs surgeon may coordinate the repair of your wound with another specialist such as a plastic surgeon, oculoplastic surgeon or hand surgeon. In most instances, however, the Mohs surgeon will repair the wound immediately after obtaining clear margins.
Step 7: Finishing up
If more than one or two rounds are needed, the entire process can take up to several hours, so be prepared for that. It’s worth it, though, because this precise technique has the highest cure rate of any treatment method and can save the greatest amount of healthy tissue, leaving the smallest scar possible. Carefully follow your doctor’s instructions for wound care, scar care and follow-up to achieve the best outcome.
Is Mohs right for me?
Mohs surgery is the gold standard for treating many basal cell carcinomas (BCCs) and squamous cell carcinomas (SCCs), including those in cosmetically and functionally important areas around the eyes, nose, lips, ears, scalp, fingers, toes or genitals. Mohs is also recommended for BCCs or SCCs that are large, aggressive or growing rapidly, that have indistinct edges, or have recurred after previous treatment. Some surgeons are also successfully using Mohs surgery on certain cases of melanoma.
Get more information about Mohs surgery.