By Deborah S. Sarnoff, MD
“Dr. Sarnoff, are you aware that you have a black spot on your scalp?” asked Manolita, the woman washing my hair. I was in the same chair, at the same salon with the woman who, for the past 25 years, has washed my hair during my monthly hair appointments.
“It’s not washing off,” Manolita said. Then she held up a mirror for me.
“I can’t see anything,” I replied. Two mirrors didn’t help. Suddenly I had an idea: “Can you take my cell phone out of my purse and snap a photo for me?”
Looking at the photo on my iPhone, I started trembling. I almost fainted right there in the chair.
The lesion had most of the classic ABCDE warning signs of melanoma: asymmetry, irregular borders, variegated colors (from dark brown to jet black), a large diameter and dark in color. The E is for evolving or changing, but since this was the first time I’d seen this spot on my scalp, I didn’t know its history. Beginning to panic, I told Manolita, “Please rinse out the shampoo and forget the haircut. I’ll come back another time.”
I immediately called my husband, Robert Gotkin, MD, a plastic surgeon who shares an office with me, and told him “Please meet me at the office right away. I need to have this spot excised immediately. What if it’s a melanoma?” I shuddered to think it, because scalp melanomas are the most lethal of all melanomas.
It dawned on me how utterly ironic it was. I’m a dermatologist and president of The Skin Cancer Foundation, someone who regularly touts the need for monthly head-to-toe skin self-examination. I always perform the most meticulous total-body exams on my patients — including the scalp. I’m also a Mohs surgeon and operate on more than 1,000 patients who have skin cancer every year. And yet, I’d had no idea there was a potential melanoma on my head. How could I have neglected to check my own scalp?
The truth is, it can be tricky to see your scalp. Using a mirror and a blow dryer can help. So can asking a partner, friend — or hairstylist — to look and take photos if needed. But I had never asked anyone to look for me before.
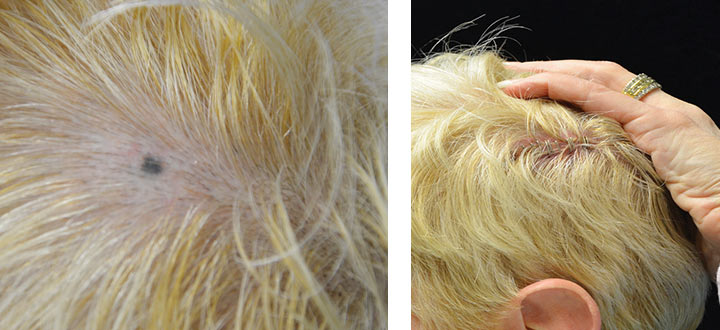
You can’t tell by looking at the photo of my scalp (above left) if my spot is a skin cancer or not, but a biopsy can determine that. The photo above right shows my scalp after the biopsy.
The next few days were the longest of my life as I anxiously awaited the results of the biopsy. Finally, a call from the lab. The verdict? “It’s benign!” Those are the two best words you ever want to hear. Turns out, it was a blue nevus, a totally benign pigmented lesion that mimics the appearance of melanoma.
Overjoyed, I purchased gift certificates for the staff at the hair salon and headed straight to the salon to give thanks and praise for what they had done. Then and there, I vowed to share my experience and good fortune, and to spread the word about scalp melanoma and the important role hairstylists can play.
The Deadliest of all Melanomas
Melanoma is derived from melanocytes, the skin’s pigment cells, and can spread quickly (metastasize) through the lymph nodes or bloodstream if not detected at an early stage. Scalp melanomas are more lethal than other melanomas. A 2014 study found that melanomas on the scalp have a much higher incidence of spreading to the brain (12.7 percent within five years after diagnosis) than those elsewhere on the head and neck (6.7 percent), or on the trunk or limbs (4.7 percent).
Why are scalp melanomas more lethal? One reason may very well be a delay in diagnosis because of their location, in an area usually hidden by hair, where one cannot see them without some effort. And the biology of the melanoma itself or the environment of the scalp may play a role. The scalp is well vascularized with numerous blood vessels, and the lymphatic drainage is varied and complex, which may be why melanomas in this location are more aggressive and can more easily spread to the brain. A 2015 study showed that melanomas on the head and neck have a faster mitotic rate (growth rate) than melanomas elsewhere on the body.
How Can Hairstylists Help?

Here I am (third from left) with my heroes from the hair salon (left to right): Manolita Lorenzo (shampooer), Georgia Megaris (colorist) and Tasso Megaris (stylist).
Hair professionals are in a unique position to detect skin cancers on the scalp because they have a natural view of difficult-to-see areas during a salon visit. They also see their clients on a regular basis, often at monthly intervals, and may frequently discuss health-related topics, such as wellness, illness, diet and medical care.
A 2018 article in JAMA Dermatology found that educating salon professionals about melanoma risk can be beneficial. Previous studies have shown that hair professionals are willing to speak up when they notice a suspicious spot, and the more knowledge they have about skin cancer, the more helpful their input can be.
My Advice to You
To anyone who works in a salon setting: If you see something, say something! Anything new, changing or unusual — lesions, spots, bumps or funny-looking moles — should be brought to the client’s attention. Feel free to take a photo with the client’s cell phone or point out the area in a mirror. Don’t worry about offending your clients, but try not to alarm them, either. Simply point out the suspicious-looking spot, then suggest they have a dermatologist look at it. This could be lifesaving advice.
If you are a client, don’t be afraid to ask your hairdresser, barber or shampooer to take a look at your scalp and tell you if you have any unusual spots. If you do, have them checked out promptly by a dermatologist. Be sure to wear a hat in the sun to protect the scalp from the sun’s harmful ultraviolet rays.
Deborah S. Sarnoff, MD, is a clinical professor of dermatology in the Ronald O. Perelman Department of Dermatology at NYU School of Medicine in New York City. Cofounder and codirector of Cosmetique Dermatology, Laser & Plastic Surgery LLP, a private practice in Manhattan and Long Island, Dr. Sarnoff is also president of The Skin Cancer Foundation.





