Bill Ridenour with his family
Skin Cancer Foundation staff members learn a lot about skin cancer. Many of us also have friends or family members who have suffered from the disease. However, few of us have developed the disease ourselves. Bill Ridenour, the Foundation’s senior director of partnership development, recently became part of that small group.
A Sun Guy
Bill joined the Foundation in the fall of 2016 to oversee the corporate partnerships department. His switch to the non-profit sector came after 30 years of working in the advertising industry, at publications like Time, Sports Illustrated, Fortune, Money and Golf Digest.
By his own admission, Bill grew up spending a lot of time outdoors, and sun protection was never a priority. An avid golfer, boater and tennis player, Bill says he was always happiest lying on the beach in the sun. “I have been a ‘sun guy’ for…forever.”
When asked if he had ever visited a dermatologist, Bill recalls appointments as a teenager to treat acne. Until March 2017, he had never had a professional skin exam.
Divine Intervention

Dr. Perez and Bill in her office
Bill had been working at The Skin Cancer Foundation for just a few months when he met Maritza Perez, MD, at a Foundation event in Orlando. Dr. Perez is a dermatologist and one of the Foundation’s senior vice presidents. Her practice is in New Canaan, Connecticut– very close to Bill’s hometown of Greenwich. As they chatted, he mentioned a small bump on the side of his head that he suspected was a cyst. “Call my office to make an appointment and I’ll take a look,” Dr. Perez said.
Bill took Dr. Perez’ card and flew home. Several weeks went by before his wife, Susan –who was worried that the bump on his head could be serious– reminded him to make an appointment.
The day of his appointment, a Friday, Dr. Perez looked at Bill’s head and diagnosed a benign (noncancerous) pilar cyst. Bill would need to make another appointment for her to remove it.
He was about to leave when she offered to give him a full-body skin exam.
“I always offer a skin exam to my new patients,” says Dr. Perez. “My motto is, ‘if you don’t check, you don’t find.”’
Using a dermatoscope –a handheld magnifier specifically used to examine the skin– Dr. Perez carefully examined Bill’s face, mouth, scalp, shoulders, chest and arms. Then she turned him around to look at his back…and got very quiet.
“I don’t like what I’m seeing,” she told him. Dr. Perez had spotted what she was certain was melanoma, and what she feared on closer visual inspection was an invasive melanoma. In fact, she spotted two lesions: one on his lower back that was particularly concerning, and a smaller lesion on his upper back.
According to Dr. Perez, Bill’s melanomas had some of the classic characteristics of the disease. Both lesions had irregular borders and were a variety of colors. They also showed signs of regression, meaning the lesions showed signs that part of the melanoma had been destroyed by Bill’s immune system and replaced by scar tissue. When regression is evident, the total size of the melanoma is hard to characterize because it is difficult to tell how extensive it was before the regression occurred.
Dr. Perez biopsied both lesions that day, and sent the samples to the lab. There was nothing to do but wait for the results.
The Waiting Game
Bill had woken up that morning believing he would have a cyst removed; he did not expect to be told he likely had two melanomas. He returned home, with Dr. Perez’ words running through his mind. Susan came home to find Bill sitting alone in their family room, still processing the news. Later, she would tell him he had “the look of death” on his face.
“You immediately think the worst,” says Bill. “I thought I was going to die.”

Bill’s stage IA melanoma
Bill returned to work the following week after a long weekend spent worrying about the results. He was staring at his computer, trying to focus when Dr. Perez called with the results. “I have good news,” she told Bill.
The lesion on his lower back was stage IA melanoma– what’s referred to as a “thin melanoma.” Although the melanoma had invaded below the epidermis (the skin’s outer layer), it was unlikely that it had spread beyond the tumor site. The lesion on his upper back was melanoma in situ, meaning the tumor had not penetrated beyond the epidermis.
Dr. Perez told Bill to come to her office the next day to remove the invasive melanoma. Both tumors would need to be completely removed and sent to a lab, to confirm they had not spread.
The Procedure
To remove Bill’s thin melanoma, Dr. Perez used a technique called “slow Mohs.” Like traditional Mohs surgery, the slow Mohs technique allows as much healthy skin to be spared as possible. When performing Mohs surgery, the surgeon removes a thin layer of tissue, which is then frozen and immediately examined under a microscope. If the margins of the tissue have no signs of cancer the surgery ends. Otherwise the surgeon repeats the process until the tissue margins show no cancer. Mohs surgery is considered the gold standard of treatment for nonmelanoma skin cancers (basal and squamous cell carcinomas), which can freeze quickly and are easy to read. But because melanoma is made up of the pigmented skin cells (melanocytes), they are harder to read. With slow Mohs, the tissue sample is removed using a technique similar to traditional Mohs, but must be sent to an off-site pathology lab for more complex analysis.
Bill’s thin melanoma was removed, and he was sent home with the wound left open, in case the pathology report indicated that a second procedure was needed.
“About 91 percent of cases are cured by the first surgery, but in about nine percent of cases you have to go back and take more skin,” says Dr. Perez.
Dr. Perez sent the lesion off to the lab, and once again it was time for the waiting game. In the meantime, Bill began to reach out to friends, family and colleagues, letting them know what he was going through. One of his friends even e-introduced him to an industry colleague who had also experienced melanoma. Although they had never met, that person became a lifeline for Bill over those next few days. “Call me every day,” he told Bill. “I know what you’re going through, I’ve been there.”
Bill calls him “the closest friend I’ve ever had whom I’ve never met.”
—
A few days later, Dr. Perez called Bill with the results: The cancer was completely gone, and there were no signs that it had spread.
“This had to be divine intervention,” Dr. Perez told Bill. If Bill had not joined the SCF team, if he had not met Dr. Perez and discovered their geographic proximity and if his wife hadn’t reminded him to make the appointment, it’s possible Bill’s melanomas would have gone untreated and potentially become fatal.
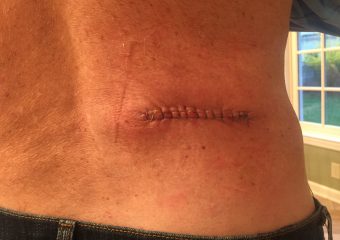
What 56 stitches looks like
Once again, Bill headed to Dr. Perez’ office so she could close the incision. The removal of approximately 4 square centimeters of skin required 56 stitches. She also removed the melanoma in situ –a 12 millimeter lesion– and closed that wound with 32 stitches.
“The stitches were definitely uncomfortable,” says Bill. “You don’t realize how much you stretch your back muscles until you’re trying not to.” It was a few weeks until he could resume his normal, active lifestyle. Still, he considers the discomfort and inconvenience a small price to pay for his life.
Moving Forward
Since Bill’s diagnosis, his wife and three adult children have all visited Dr. Perez for skin cancer screenings. He describes his family as “former sun worshippers” who are now “all in” when it comes to staying sun-safe.
Now Bill has a whole new approach to sun protection. On a recent family beach trip, instead of lying out on the sand as he used to, he spent the day underneath an umbrella. His extended family, surprised, asked him about his change in behavior. In response, he turned around and showed them the scars on his back.
He has a specific set of instructions from Dr. Perez to follow, too: “Bill needs to check his own skin on a weekly basis, and come in every three months for a skin check.” Although testing revealed his original tumors are unlikely to recur, she cautions that Bill is still at an increased risk for developing new skin cancers, and will need to remain vigilant.
A New View
Bill says he now has a different perspective on the Foundation’s work and its efforts to educate the public about skin cancer prevention and early detection. “I have a vested interest that I didn’t have before,” he says. “When I talk about the Foundation’s mission to save lives, my pitch is coming from the heart. It’s still so recent that when I start talking about it, I get a little emotional.”
He’s also using his story as a cautionary tale. “I have so many friends who grew up just like I did, spending so much time outdoors without sun protection,” Bill says. “I tell them my story and they say, ‘I’ve got to go get screened.’”





