Rethinking the Alphabet: Some experts believe “dark” may be an even more important warning sign of melanoma than “diameter” and deserves more awareness. Photo: baona/iStock/Getty Images Plus
Q: One of my favorite tools on The Skin Cancer Foundation website is the “ABCDEs of melanoma.” Recently I noticed that under “D” you now include, in addition to “diameter,” a second warning sign for “dark.” What prompted this change, and what does it mean in terms of the checks I routinely do on my own skin?
Elizabeth K. Hale, MD: The Skin Cancer Foundation did a huge service to medical practitioners as well as the general public back in 1985 when it gave an international platform to the now well-known acronym “ABCDs of melanoma,” later expanded to the ABCDEs. For nearly four decades, this simple, alphabetized list of warning signs from A (“asymmetry”) to E (“evolving”) has given consumers a simple, easy-to-remember way to perform a thorough inventory on any worrisome spot or mark on their skin. This tool has undoubtedly helped save many lives.
As a longtime officer of The Skin Cancer Foundation, I recently advocated for the decision to amend the advice under “D” by adding “dark” as an equally — or, arguably, even more — important warning sign as “diameter.” A lot of that advocacy grew out of the conversations and correspondence I had on this topic with Georgia dermatologist Stuart M. Goldsmith, MD, who has been at the forefront of this initiative.
Stu reached out to me because he’d seen YouTube videos of my lectures to medical students in which I expressed my concerns about the “diameter” criterion. Many melanomas are tiny, and a melanoma that reaches a diameter of 6 millimeters (about the size of a pencil eraser) has often already advanced beyond the optimal stage for treatment. As with any cancer, the earlier it’s detected, the better. Also, many types of lesions that can typically be greater than 6 mm are perfectly benign. So “diameter” may not be as meaningful, especially since we have gotten much better at diagnosing early and smaller melanomas [see photos below].
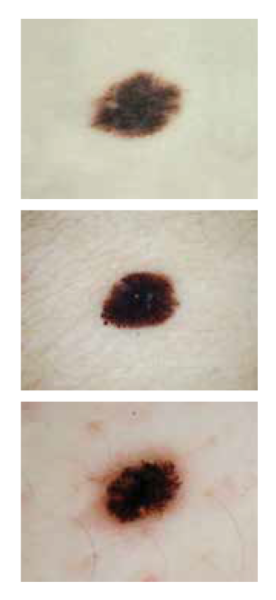
Dark and Small: The three melanomas above were all diagnosed at around 4 millimeters in diameter, with each displaying distinctive darkness. Lesion photos: International Skin Imaging Collaboration at isic-archive.com
Stuart M. Goldsmith, MD: Exactly. Over the many years I studied this, the primacy of “dark” in detecting melanomas made far more sense to me than “D is for diameter.” So kudos to The Skin Cancer Foundation for taking the lead in recently making that change. After all, the very word “melanoma” derives from the Greek melanos (black) and oma (tumor). While certainly not all melanomas are dark — and a rare type of amelanotic melanoma can be a nearly colorless faint pink — most melanomas are dark somewhere.
Moreover, melanomas usually occur on light skin. Even in people with darker skin, where lower rates of melanoma carry higher rates of mortality than among lighter-skinned people, melanomas often occur on less pigmented skin, such as the palms of the hands and the soles of feet. In other words, because the eye perceives contrast, the most important feature — darkness — is also the easiest to see. Quite simply, it needs to be at the center of skin cancer education. And historically, it has not been. I believe education regarding melanoma must emphasize how important it is to look for any lesion that stands out for being dark.
Medicine has an academic tradition of emphasizing exceptions. In cardiology, for instance, chest pain is the most common symptom of heart attack, but not all heart attacks involve chest pain. My own father had three heart attacks with zero chest pain, for example. So I know that awareness is vital. Even so, chest pain unquestionably must be at the top of the list of warning signs. Similarly, in dermatology textbooks, the focus on amelanotic melanoma, which is exceedingly rare, has often been disproportionate to its probability. Sure, textbook descriptions of melanoma usually include the fact that most are black or dark brown. That is not new information. My point is that darkness is a main feature of melanoma and as such deserves center stage.
I’ve even wondered if the redundancy of the diameter criterion might move more dermatologists to, perhaps, consider dropping it. Say you have a lesion of 6 millimeters in diameter. By the time you figure that out, your spouse talks you into seeing a doctor, you make an appointment and you get time off work, that lesion will be 8 or 9 millimeters. That’s no way to diagnose early melanoma. In any case, no doctor would excise a lesion solely because of its 6 millimeter diameter; there has to be some other indication that the lesion may be cancerous. As Liz notes, many larger spots can be benign.
EKH: I agree with most of what you say, Stu, but I don’t believe we should jettison “diameter” from the ABCDEs yet. For now, I think it’s best to keep both D’s. But as we continue to think about this, it’s important to point out how much better our profession has gotten at diagnostics. With the advent of dermoscopy, a technique that allows us to evaluate pigmented lesions with a microscope applied to the skin, along with the insights into melanoma that we’ve gained over the past 20 years, dermatologists have gotten much better at diagnosing smaller melanomas. So it’s less common for a melanoma to get to the classic 6 millimeters in size. A more fundamental question around the issue of “diameter” is whether a lesion is growing rapidly, which might raise a red flag. But as Stu says, a lesion that’s very dark, whether it is new or changing, is much more likely to be melanoma than something that happens to be greater than 6 millimeters in diameter.
That said, I do want to stress that lesions do not have to be very dark to be melanoma. While a lesion that is homogeneously black is instantly concerning, I see many more melanomas that have variations in color — some brown, some light brown, some darker brown. And yes, even some of the rare melanomas lack pigment altogether. That’s why all the other criteria in the ABCDE acronym remain important and should be used in conjunction with “dark.”
SMG: About the various colors, I agree with Liz that a lot of melanomas cannot be described as uniformly dark. Still, there is usually relative darkness within them. Part of the value of darkness as a marker is the recognition that it’s not an absolute: a lesion may be dark for that particular patient, or there may be a variation within a lesion that creates a contrast between lighter and darker. For instance, even when neither side is particularly dark, you would still use the term “darker” to describe one side over the other. The term is still useful. And often, when you examine the lesion further, some of the other ABCDEs come into play. It may also be asymmetrical, have an irregular border or have changed. So while “dark” is a crucial marker in and of itself, it’s important to understand that it also enhances the applicability of the other features of melanoma.
Another important adjunct to the ABCDE list is the “ugly duckling” warning sign: an atypical mole that sticks out among, and looks different from, its neighbors, or appears all by itself in isolation, without neighbors. Basically, you need to peruse the various marks and spots on your skin, looking for the atypical among them (or “unusual,” as in the Foundation’s Big See campaign, which teaches the public to look for anything “new, changing or unusual” on their skin). In fact, when it comes to the ABCDEs, eventually we could consider changing “diameter” to “different” under “D”: How about “D is for dark and different”?
EKH: That’s an interesting idea to consider for the future! As to the question of what patients can do with this new information, I would encourage them to incorporate the “D is for dark” marker for melanoma into their careful skin checks as advised by dermatologists and organizations like The Skin Cancer Foundation. Like Stu, I firmly believe that darkness should be front of mind during these checks. If you have, say, a new black lesion or, especially, a nodule that is very dark, it may well meet some of the other criteria such as asymmetry or irregular borders. But it may share none of those characteristics. Perhaps it is not asymmetric, does not have an irregular border and lacks any variability within it. In short, it may match none of the usual signs of a possible melanoma. But it is very dark, and, to Stu’s point, it is “different” in that it is new.
In such a case, I cannot stress this enough:
It is essential to realize that darkness is a characteristic that can stand alone as a warning sign of melanoma and that no other warning signs need to be present for it to require prompt evaluation.
No other warning signs need to be present. You should waste no time in calling your dermatologist to be evaluated for a possible biopsy. — Interview by Lorraine Glennon
About the Expert:

Elizabeth K. Hale, MD, is a board-certified dermatologist, cofounder of CompleteSkinMD and a clinical associate professor of dermatology at NYU Langone Medical Center. She specializes in Mohs surgery, cosmetic dermatology and laser surgery and is a senior vice president of The Skin Cancer Foundation.

Stuart M. Goldsmith, MD, is a board-certified dermatologist in private practice in Albany, Georgia. He has a volunteer association with the departments of dermatology at Florida State University College of Medicine and Emory University School of Medicine. He is a past president of the Georgia Society of Dermatology and Dermatologic Surgery.






