Illustration by James Yang
Diagnosing skin cancer is a visual process. The trained eyes of a dermatologist have long been the state of the art. But technological advances are showing that digital tools hold a promising future to help doctors achieve earlier and more accurate skin cancer diagnoses — and engage patients to take a more active role in their own care. In part 1, we look at total body scanners. In part 2, we see how technology is evolving to help diagnose skin cancers at their earliest, and most curable, stages. Part 3 looks at virtual visits and how to secure your valuable medical data.
By Dan Ferber
Gary Wiemokli was about to step into what looked like a spaceship. It was May 2017. Dermatologist Michael A. Marchetti, MD, an expert in melanoma management at Memorial Sloan Kettering Cancer Center, knew that Wiemokli was at high risk for this dangerous skin cancer and had recommended he get checked out by a futuristic new diagnostic tool.
As a teenager in the Southern California town of Encinitas in the late 1960s, Wiemokli had surfed off Moonlight Beach, and during the summers he worked there as a lifeguard. “I was in the ocean probably 40 hours a week,” he recalls. Despite having pale skin and strawberry-blond hair, Weimokli didn’t see sun protection as a priority. “In the 1960s and 1970s, you put zinc on your nose and relied on good luck for the rest of you.”
His luck changed in 2015. Then living in Connecticut, Wiemokli noticed a black growth on his knee. At Baystate Hospital in Springfield, Massachusetts, he had the growth, a wide margin of bordering tissue and nearby lymph nodes removed. His lymph nodes were clear, showing the disease had not spread, and he was diagnosed with stage II melanoma. It’s a good thing he got it checked then, or it could have been worse.
Then Wiemokli learned that patients like him, who have light skin, lots of moles and have been diagnosed with one melanoma, are at risk for others — or a recurrence. He would have to be vigilant and see a dermatologist every few months. He decided to go to New York City for specialized care, where he met Dr. Marchetti. “He has so many moles, I recommended total-body photography,” Dr. Marchetti says. Not long after, Wiemokli took off his robe and stepped into the large spaceship-shaped scanner. (Yes, for best results you should be naked, but the staff is highly professional, respectful and discreet.)
In a single flash of light, the 92 digital cameras embedded in the scanner’s frame snapped high-resolution photos, capturing 95 percent of Wiemokli’s body surface. The scanner’s advanced image-processing software then stitched these images into a 3-D avatar of his body. It incorporated close-up images of worrisome moles as well, so a clinician viewing the avatar could zoom in on them for a more detailed look.
When Wiemokli returned three months later for a follow-up, Dr. Marchetti checked to see if any moles had changed, comparing the moles on his patient with those on the avatar from the initial visit. A spot on his chest had changed, ever so slightly, becoming discolored with an irregular border. It didn’t look like much to Wiemokli; he had barely noticed it. But the doctor, with high-tech help from the machine, was concerned.
Dr. Marchetti did a biopsy of the mole and sent the tissue to a lab for analysis. The biopsy revealed that the spot on Wiemokli’s chest was melanoma in situ, the earliest form of melanoma you can identify. As soon as it could be scheduled, a surgeon cut out the tumor and a safe margin of skin, then closed the wound.
Two years later, Wiemokli is “doing phenomenally well,” Dr. Marchetti says. He’s enjoying retired life in Connecticut, tooling around the countryside with his partner, Karen, in his 1929 Model A Ford, and playing bass and six-string slide guitar in a couple of classic-rock bands. He continues to get regular checkups with his dermatologist. He wears a hat and sun-protective clothing. “And I’ve become the street-corner preacher for wearing sunscreen,” he says with a smile.
It’s All About “Seeing”
Skin cancer grows on the outside of the body, and while it seems like cancer would be obvious, it can be very subtle. Suspicious skin lesions may be noticed first by a dermatologist during a skin screening or an appointment for another skin issue. Others may first be noticed by patients themselves or their family members, or by primary care providers, who may refer the patient to a dermatologist. With their special training, dermatologists look closely at suspicious lesions. They might snap close-up digital photos with a dermatoscope, a handheld, low-magnification microscope that visualizes the outer surface of the skin (the epidermis) and the layers just beneath it. Next, they may decide to perform a biopsy on a skin lesion that looks worrisome and send the tissue to a laboratory to check for cancer. These procedures help detect melanoma and other skin cancers in their earliest stages, while cancer is confined to the skin’s outermost layer.
Dermatologists have the most training and experience at recognizing the early signs, but with more than 5.4 million cases of skin cancer in the U.S. each year (about 190,000 of which are melanoma), they could use some help. Total-body scanners like Sloan Kettering’s, a Vectra WB360 machine from Canfield Scientific, are still very rare, but they can provide state-of-the-art data for dermatologists whose patients are at high risk for melanoma. They are not a substitute for an experienced dermatologist, but they may enhance the doctor’s diagnostic skills. And more than likely, they offer a glimpse of the future of skin cancer diagnosis.
“Because dermatology is a visual specialty, it’s a given that advances in imaging will bring enormous value,” says Allan C. Halpern, MD, chief, Dermatology Service, at Memorial Sloan Kettering in New York City. But when this will be widely available is another question.
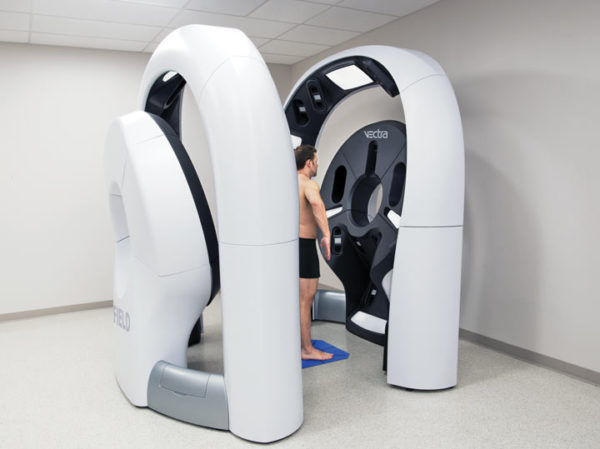
They look futuristic, but total-body scanners help dermatologists track evolving moles over time: Doctors can rotate a 3-D avatar of the patient and quickly spot and zoom in on menacing moles. Photo credit: Canfield Scientific
Dan Ferber is a journalist based near New York City and a former editor at Discover magazine. He writes about science, medicine and other topics for national publications.

*This article was first published in the 2019 issue of The Skin Cancer Foundation Journal.





