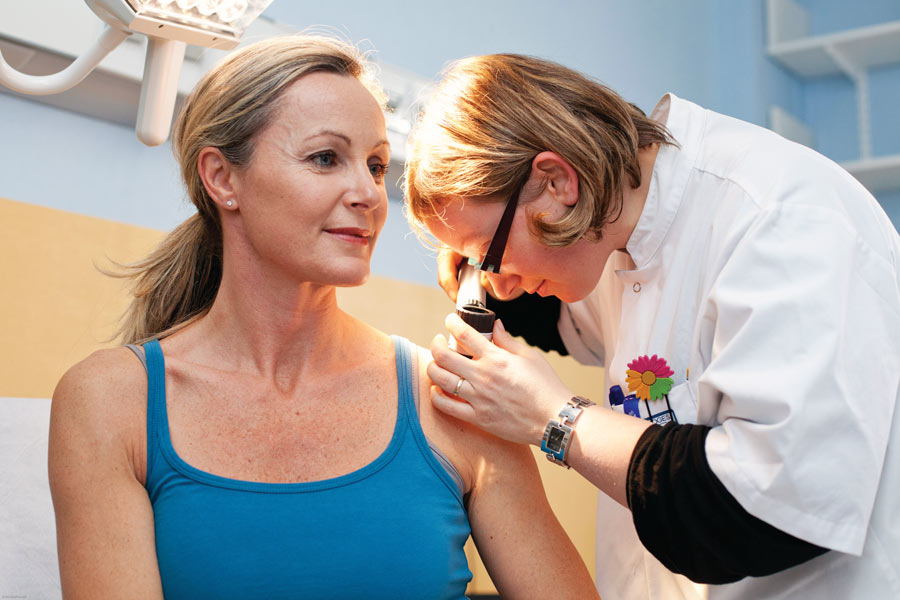
No matter how much technology improves, there’s still no substitute for regular visits with a dermatologist. Some precancers and skin cancers may be identified by texture, as well as a doctor’s experience and intuition.
Diagnosing skin cancer is a visual process. The trained eyes of a dermatologist have long been the state of the art. But technological advances are showing that digital tools hold a promising future to help doctors achieve earlier and more accurate skin cancer diagnoses — and engage patients to take a more active role in their own care. In part 1, we looked at total body scanners. In part 2, we see how technology is evolving to help diagnose skin cancers at their earliest, and most curable, stages. Part 3 looks at virtual visits and how to secure your valuable medical data.
By Dan Ferber
For decades, forward-looking dermatologists had been dreaming about using computer vision and artificial intelligence (AI) to help diagnose and monitor potentially deadly skin cancers. But for just as long, AI was not up to the task. Computers once “thought” in a rote, linear manner, “like the simple, programmable systems you still have in your refrigerator,” says Harald Kittler, MD, a professor of dermatology at the Medical University of Vienna, whose research has focused on digital dermoscopy and pigmented lesions.
But beginning around 2012, computers began mastering complex skills that they’d never mastered before, thanks to an avalanche of advances (some from the video-game industry). These led to breakthroughs in neural networks — computer programs modeled on the way the human brain works. Today these networks learn from experience the way children do. “We used to tell the computer what to do, but giving it rules didn’t work so well,” says Allan C. Halpern, MD, chief, Dermatology Service, at Memorial Sloan Kettering in New York City. “Now we train AI the way we train kids.”
As children learn by trial and error, neurons in the brain connect with each other to form circuits. Circuits that produce correct or useful answers are strengthened, while those that lead to incorrect or unhelpful answers are weakened. While learning, our brains are rewired. Machines’ neural networks that learn this way could train themselves without human help by recognizing patterns in real-world datasets. As they’ve evolved, they’ve gotten faster and better. They have defeated world-class masters in complex games like the abstract board game Go. They have recognized voices and transcribed human speech. And they’ve made computer vision and human facial recognition reliable enough to be used in law enforcement and even in smartphones.
Encouraged by these advances, in 2015 Dr. Halpern and a team of collaborators created a project called the International Skin Imaging Collaboration (ISIC) as a worldwide effort to reduce melanoma mortality by using digital skin imaging in new ways.
Challenging the World to Help Diagnose Melanoma
Job number one for ISIC was to assemble a large public set of quality-controlled dermoscopic images of skin lesions that could be used to train both humans and software. It was no small task. Under the umbrella of the International Society for Digital Imaging of the Skin, Dr. Halpern enlisted leading dermatologists, including Harald Kittler, MD, a professor of dermatology at the Medical University of Vienna, whose research has focused on digital dermoscopy and pigmented lesions, as well as others in Australia, Spain, Colombia and elsewhere. Together, they assembled more than 12,000 close-up images of both harmless moles and melanomas that had been collected in clinical exams. “Just setting up the archive of images and putting it in the public domain was a huge accomplishment,” Dr. Halpern says. Next, he and his colleagues spoke and held workshops at leading medical imaging conferences to engage the computer science community. “That was another huge challenge.”
Then ISIC created a competition that kicked off in the spring of 2016. They challenged computer scientists worldwide to use ISIC images to develop computer models that could help diagnose melanoma. By April, 25 teams of computer scientists were competing in the ISIC Challenge. Each team built an app and then helped it “learn” with a training set of 900 images. After the apps were trained, the competing teams evaluated them on a separate test panel of 379 images. Eight dermatologists who specialize in skin cancer analyzed the same test panel. The computer vision apps proved more accurate than some, but not all, of the dermatologists.
Encouraged, Dr. Halpern and his colleagues repeated the competition in 2017 and again in 2018, making the challenge harder each time. In the computer science world, a competitive fever took hold. By September 2018, 130 teams of app builders had taken the ISIC Challenge. Not to be outdone, more than 500 clinicians got into the game as well. The algorithms did better than ever before, outperforming clinicians 96 percent of the time at diagnosing melanoma. While this technology is not ready for prime time in doctors’ offices nationwide, “It was proof of principle that a computer can definitely help dermatologists with the diagnosis part of their job,” says Dr. Halpern.
Human Versus Machine?
As digital imaging, automation and machine intelligence improve at breakneck speed, some dermatologists worry about how it will affect them and their practices. “They feel threatened, but they shouldn’t,” Dr. Kittler says. The endgame is not a match of humans versus machines, he explains. Instead, digital tools will improve dermatologists’ ability to care for their patients. They’ll enable doctors to make a diagnosis more easily, help prevent unnecessary procedures and enrich the dermatologist-patient experience.
Whether or not dermatology welcomes them, changes are coming, as part of a broader wave of innovation sweeping across the medical profession. “Current paradigms of health-care delivery are in flux, which is both a challenge and an opportunity,” Dr. Halpern says.
“Patients are empowered with more information and the ability to communicate with us using images,” he says. Care by advanced practice providers such as nurse practitioners and physician assistants is on the rise. So is the use of telemedermatology, which is long-distance interaction with your doctor using audio, visual and data communication. Pharmacy chains have begun to offer clinics and compete with private medical practices, as have telemedicine companies that are unaffiliated with a specific health-care system.
Meanwhile, economic changes are afoot, as small group providers are incorporated into larger groups or major medical systems, which are themselves being bought up by venture capitalists. All these changes mean pressure will increase to use technology to reduce costs and increase profits.
These changes will not occur quickly or easily, and the profession has a lot of work to do, Dr. Halpern says. “We should figure out how to leverage digital imaging and mobile technology while medicine is transforming and determine the best ways to take greatest advantage. If we do that optimally, we should be able to do a much better job of delivering health care. We’re pretty close to a tipping point where we’re going to see real changes.
Dan Ferber is a journalist based near New York City and a former editor at Discover magazine. He writes about science, medicine and other topics for national publications.

*This article was first published in the 2019 issue of The Skin Cancer Foundation Journal.