Daisy Mae the puppy visits James in the hospital during his first bout with sepsis. Photo: Jamie Gentry
Jamie Gentry’s husband, James Gentry, had been talking about losing weight for years when he shed 25 pounds over a few months in 2017. James suggested the transformation could be a result of his own efforts, but Jamie was unconvinced — and deeply concerned.
“He’s a big man, and ever since I met him he’s been talking about losing weight,” Jamie says, chuckling. “Never changes what he does or what he eats, but he was going to lose the weight. I said, ‘No, no, you’ve been trying for 12 years; it’s not suddenly working.’ It really freaked me out.” Jamie’s instincts were spot on — she knows now, two years later, that a rapidly metastasizing Merkel cell carcinoma (MCC) was the reason for James’ sudden weight loss.
But back in May of 2017, no one seemed to know much about the lump James, then 59, noticed on his leg. It took several visits to his primary care physician and his cardiovascular surgeon (who he was visiting for a pre-existing condition) to get the bump more than a passing glance. James persisted, as he had noticed the spot seemed to be getting bigger. Eventually, his physician ordered a Doppler ultrasound to investigate. The radiologist admitted to having no idea what he was seeing. James’ PCP finally decided that the tumor, “whatever it was,” should be removed.
“We’re all standing there, and James is still lying on the table having this thing cut off of his leg,” Jamie recalls. Everyone expected it to be a cyst or a blood clot — James had a history of both — but when the general surgeon excised the lump, he said he had never seen anything like it before. “Feels really good to hear the doctor say that,” Jamie quips.
The surgeon stitched up James’ wound and instructed him to come back in a week so he could have the stitches removed. Jamie didn’t accompany her husband to the appointment. She figured if the lump had been anything serious, the doctor would have called. But when James returned home, he reported that the doctor had made him sit down before telling him that the excised tumor had been a Merkel cell carcinoma (or MCC), a rare and very dangerous type of skin cancer. Five months had passed since James first tried to bring the cancer to a doctor’s attention.
A Terrifying Diagnosis
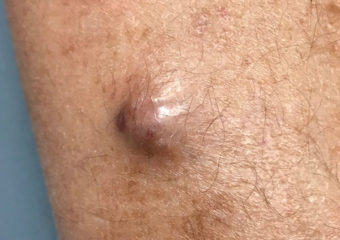
The bump on James’ leg that turned out to be a Merkel cell carcinoma. Photo: Jamie Gentry
“We had no idea what it [MCC] was,” Jamie says. “We had never heard of it. When the doctor said it was a skin cancer, we said, ‘OK…so?’”
Jamie and James immediately went online to find out more about the diagnosis. What they found wasn’t as helpful as they had hoped it would be. “Part of the frustration is that there’s not a lot of information on Merkel cell,” Jamie says. “Everything on the web is terrifying, and the more we read, the scarier it got. It all pretty much says to make your final plans. It says you’re going to die.”
Jamie’s daughter, a practicing nurse, started asking around about MCC at the hospital where she works. One of the oncology physicians called the disease “the kind of cancer that you don’t know how far it’s spread until you do the autopsy.”
After some research, the couple was able to identify Frank Saporito, MD, as the nearest MCC expert. Based in Dallas, Dr. Saporito was 70 miles south of where Jamie and James live in Bonham, Texas. He explained that while MCC is certainly nothing to underestimate, James’ situation wasn’t hopeless. “He said, ‘We know more now,’” Jamie recalls. “He said, ‘We know it doesn’t respond to chemo. We know this, that and the other thing.’ But he still said it was a good idea to get your affairs in order.”
Once James had a diagnosis, things moved along quickly, but it hasn’t been an easy journey. He underwent a sentinel lymph node biopsy, which showed the cancer had spread to four nearby lymph nodes. From there, a web of treatments and side effects has caused a long list of problems. He began radiation in December of that year. That caused complications to the wound at the original tumor site, which led to hyperbaric therapy to help close the wound. James has also dealt with bouts of sepsis, spiked blood sugar as a result of a steroid treatment, an inflamed thyroid and an enlarged heart. “If it’s not one thing, it’s another,” Jamie summarizes.
James had two new suspicious spots biopsied in February 2018, which turned out to be more MCC. This led to immunotherapy using Avelumab. “He began immunotherapy with six tumors, and five of those six were resolved,” Jamie says. “One of them kept growing, and Dr. Saporito finally removed it in November 2018.”
James returned for a new AMERK test three months later. Unfortunately, the test showed that MCC was still present — but he had no visible tumors left. James is set to visit Dr. Saporito again to determine next steps.
Using Her Voice
Jamie took an active role in James’ treatment process. One of the first things she decided was that she would accompany James to his doctors’ appointments, not only to support him but to act as an advocate when he may be unwilling or unable to do so himself.
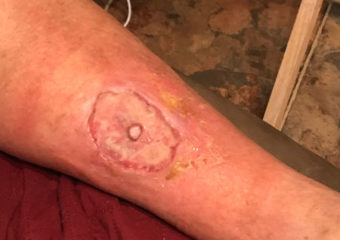
James’ leg after a skin graft. Photo: Jamie Gentry
As part of James’ wound treatment, he would go in to have his leg outfitted with a compression wrap from his toes to his knee. He developed a skin allergy to the latex used, so the wound had to be wrapped very particularly to avoid a reaction. One day he came home from treatment and Jamie saw that the nurse had wrapped his leg incorrectly. She asked why James didn’t stop her. “He said, ‘You know I won’t do that,’” Jamie recalls. “He’d rather just come home and have me fix it. So I’ve learned to wrap his leg when they mess it up. He won’t advocate for himself — you’d think that he would, but that’s why he’s not allowed to go alone anymore!”
Jamie has also noticed that she is more likely to speak up and question doctors when she notices something that doesn’t seem right. “I take notes and ask questions when we go see the doctor,” she says. “I think they’re used to people not really reading what they’re given and just going along with it. But you have to be informed to be able to make an informed decision. Question the doctors over and over until they are straight with you.”
One example is when James was given a written treatment plan for his MCC, which had at that point reached stage IV. The plan listed immunotherapy with avelumab for six months, then palliative care, then hospice. “Next time we went in there, I brought it [the treatment plan] with me and said, ‘What the heck does this mean?’” Jamie says.
The oncologist explained that the pamphlet only listed six months of immunotherapy because the insurance company would only approve six months at a time. James would likely receive the infusions for two years. Palliative care was listed to make him comfortable while waiting to see what his response would be. Of course, the doctor said, he would not have to go to hospice if he had a durable response (meaning he experienced a lasting, satisfying reduction in cancerous cells).
“But if he didn’t have a durable response and he has a recurrence, there’s nothing other than hospice at that point,” Jamie says. It was a rattling realization, and Jamie remembers James laughing — that was his way of dealing with the information. “He goes, ‘So am I going to die?’ She [the oncologist] looks him in the eye and says, ‘Only if you’re a bad driver and get in a wreck on the way home.’ How’s that for an answer?”
A New Frontier
Since avelumab is still so new (it was FDA approved in 2017), Dr. Saporito explained that it’s difficult to give a concrete prognosis. MCC may have once been a death sentence within six months to two years, he said, but now James could be looking at five years. Everyone, even the medical professionals usually looked to for answers, are still learning.
Jamie says it can be difficult not to feel depressed about such an uncertain future. “We try not to let MCC run our lives…but it’s hard,” she says. “Physically, James feels rotten, and it’s hard to keep a good attitude. My job is to not let myself get down and wallow in it with him — but to point out the positives and to plan trips to see his kids and grandkids and other distant family.”
She recalls one morning when James woke up early to head to hyperbaric treatment, 30 miles away, a trip he hates. “He was all, ‘Ugh, I need to do this again,’” Jamie says. “I told him, ‘No, you get to do this again.’ He’s the patient, he can decide not to go whenever he wants to. He can decide not to get an infusion, or not to see his cardiologist. He can make that decision, but what are those consequences? I asked if that’s what he wanted.” James went to his treatment that day.
Dealing with side effects and visits to the doctor is difficult even with the best of support systems, but MCC’s rarity adds another layer of strain to making it through a treatment journey. Jamie has some advice for anyone who receives a Merkel cell carcinoma diagnosis. “What you have to understand is that people have never heard of this cancer — and they will not understand the gravity of the situation,” she says. “You’re going to get a lot of, ‘Well, at least it isn’t the bad skin cancer,’ and, ‘At least it isn’t melanoma.’ It makes me want to scream. Whether or not I take the time to educate someone depends on if they’re worth the time and effort, honestly. Most of the time we just say, ‘You’re right, it’s not melanoma. Why don’t you look MCC up and see what you can find on the internet about it?’”
Jamie has joined a support group for cancer caregivers at the cancer center where James is receiving treatment, though she can’t make the meetings because of work. She uses their online group as a sounding board, but James is the only patient at the center with MCC. She found an online group specifically for Merkel cell carcinoma patients, where group leaders share new publications and information that comes out about the disease and its treatments. By learning everything she can about MCC and sticking by James’ side through appointments, Jamie is committed to supporting him not only as a wife, but a caregiver, advocate and cheerleader as well.
“I know he’s fighting the battle of his life, but it can feel very lonely,” Jamie says. “Like you’re fighting on your own. But information is the great equalizer, and I’m arming myself with everything I can find.”
This post is part of a patient education series made possible through a grant from EMD Serono and Pfizer. Learn more at EMDSerono.com.