Q: While all types of skin cancer are less common in people of color, their outcomes are dramatically worse. What accounts for this gap?
Skin cancers are less prevalent in nonwhite racial ethnic groups, but when they occur, they tend to be diagnosed at a later stage and, as a result, have a worse prognosis. One study, for example, found an average five-year melanoma survival rate of only 70 percent in Black people versus 94 percent in white people. Another showed that late-stage melanoma diagnoses are more common in Hispanic and Black patients than in non-Hispanic white patients.
First, there’s a lower public awareness overall of the risk of skin cancer among individuals of color. Second, from the perspective of health-care providers, there’s often a lower index of suspicion for skin cancer in patients of color, because the chances of it actually are smaller. So these patients may be less likely to get regular, full-body skin exams. And third, the places on the body where skin cancers tend to occur in people of color are often in less sun-exposed, more out-of-the-way areas, which makes detection more difficult. For example, the most common location for melanoma in patients of color is the lower extremities — the soles of the feet in particular.
Q: Does UV radiation play a role in these cancers that turn up in spots where “the sun doesn’t shine”?
We don’t fully understand the risk factors for acral melanomas — acral meaning on the hands and feet — but sun is less likely to be a factor. In melanomas on the whole, UV radiation is certainly a major risk factor, and we see plenty of UV-induced melanomas and squamous cell carcinomas in people of color, who can have a wide range of complexions, from very light to very dark. But the proportion of skin cancers that occur in non-sun-exposed sites is greater in darker-skinned populations.
Q: When you cite a lower awareness, is it just not knowing or is it misplaced faith that having more melanin in the skin is itself sufficient protection?
I think it’s both. Melanin does confer some natural protection against the risk of skin cancers from UV, but everyone, of any complexion, is still at risk for sun-related skin cancers. So yes, sometimes there’s a false sense of immunity because of increased melanin. And then there’s also just an overall lack of awareness that these cancers actually do occur in patients of color. Day in and day out, patients are shocked to learn that you can get a melanoma on your foot, in your nailbed, in your eyes or some other place that seems protected from the sun. This information is simply not well known. So we’ve got to educate people about where to look and what to look for.
Q: What other skin cancer warning signs are different in skin of color?
About 50 percent of basal cell carcinomas (BCCs) are pigmented (meaning brown in color) in darker-skinned patients. If you look at the typical photos of BCCs used in educational materials — most of which focus on light-skinnned people — you’ll see a pink, pearly growth that may or may not be crusted. What you’ll almost never see is an image of a brown, slightly translucent lesion. Yet about half of BCCs in darker-skinned patients are brown, or pigmented, and thus easier to miss.
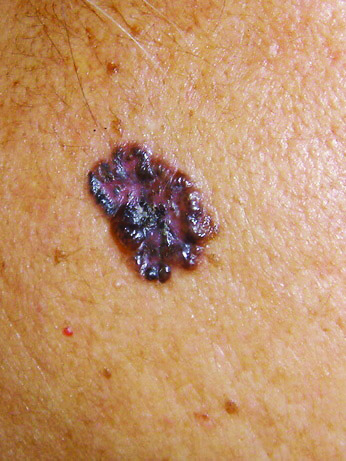
A basal cell carcinoma may be pigmented, like this one, on skin of color. Photo courtesy of Andrew Alexis, MD, MPH
Q: Prevention is key. What are the challenges?
Multiple studies show much less frequent use of sunscreen among people of color. The most important rule, as with everyone, is simply to make sure you use it. Nuances arise in helping darker-skinned patients overcome some of the aesthetic barriers to use. The mineral-based sunscreens that are least irritating often create an ashen look, with residue, and that’s a big obstacle. Patients constantly ask, “What sunscreen can I use that’s going to be acceptable for my skin?” I’ve found that the sophisticated formulations that have nanoparticles, where the zinc oxide and titanium dioxide have been micronized to limit the chalky look, tend to work well on darker skin tones. There’s been a general call to action in the industry to test sunscreen formulations on diverse populations in order to establish cosmetic acceptability across a range of skin types and complexions.
Q: One way dermatologists can often get buy-in for sunscreen use is to emphasize its antiaging properties. Is that a consideration with skin of color as well?
Exposure to ultraviolet (UV) radiation from the sun can cause fine lines, wrinkles and age spots known as photoaging. People of color generally have less severe, and also delayed, photoaging. Still, the knowledge that UV radiation accelerates skin aging has helped many patients of color see the value of sunscreen use. But the biggest motivator for patients of color is that sunscreen addresses one of their most common dermatologic concerns — hyperpigmentation (spots of excessive pigmentation). One of the best ways to manage melasma or other hyperpigmentation disorders is with sun protection. For this population, the idea that sunscreen will keep their hyperpigmentation in check makes them quite vigilant about sunscreen use.
Q: What about vitiligo, which is sort of like the flip side of hyperpigmentation in that its primary characteristic is patches of color-free skin? Is the risk of cancer greater in those white patches?
About 150,000 Americans are treated annually for vitiligo. While the condition affects people across all ethnic groups worldwide, it is of course more visually obvious in people of color. Vitiligo patients are at higher risk for sunburns, but their rates of melanoma and nonmelanoma skin cancers are lower than would be expected. That’s not to say that people with vitiligo won’t get skin cancer, but the likelihood is no greater than among the population as a whole, thanks to various immunologic and genetic factors.
Q: What other skin cancer precautions do you recommend to patients of color?
I constantly stress the importance of monthly self-examinations of the skin that include not just sun-exposed areas but also the soles of the feet, the palms, the toenail and fingernail beds and also the genital areas — places that one might not even think to look. That’s really where the biggest learning gap is. And everyone should get a full-body examination from a dermatologist once a year — or any time they see something unusual, such as a new or changing growth or mole or, particularly in skin of color, a sore that doesn’t heal. Unfortunately, most people of color are not doing this.
However, I’ve observed growing awareness of the dangers of skin cancer among populations of color. We have a long way to go, but the interest is there. I think in the next phase we’re going to see larger-scale change that results in actual reduction of some of the disparities. I’m very optimistic about the future. — Interview by Lorraine Glennon
About the Expert:
 Andrew Alexis, MD, MPH, is chair of the Department of Dermatology at Mount Sinai St. Luke’s and Mount Sinai West in New York City. He is also professor of dermatology at the Icahn School of Medicine at Mount Sinai. As director of the Skin of Color Center in New York City, he is actively involved in advancing patient care, research and education pertaining to dermatologic disorders prevalent in ethnic skin.
Andrew Alexis, MD, MPH, is chair of the Department of Dermatology at Mount Sinai St. Luke’s and Mount Sinai West in New York City. He is also professor of dermatology at the Icahn School of Medicine at Mount Sinai. As director of the Skin of Color Center in New York City, he is actively involved in advancing patient care, research and education pertaining to dermatologic disorders prevalent in ethnic skin.






